Ankle fracture: Posterior malleolar fixation using a posteromedial approach
Overview
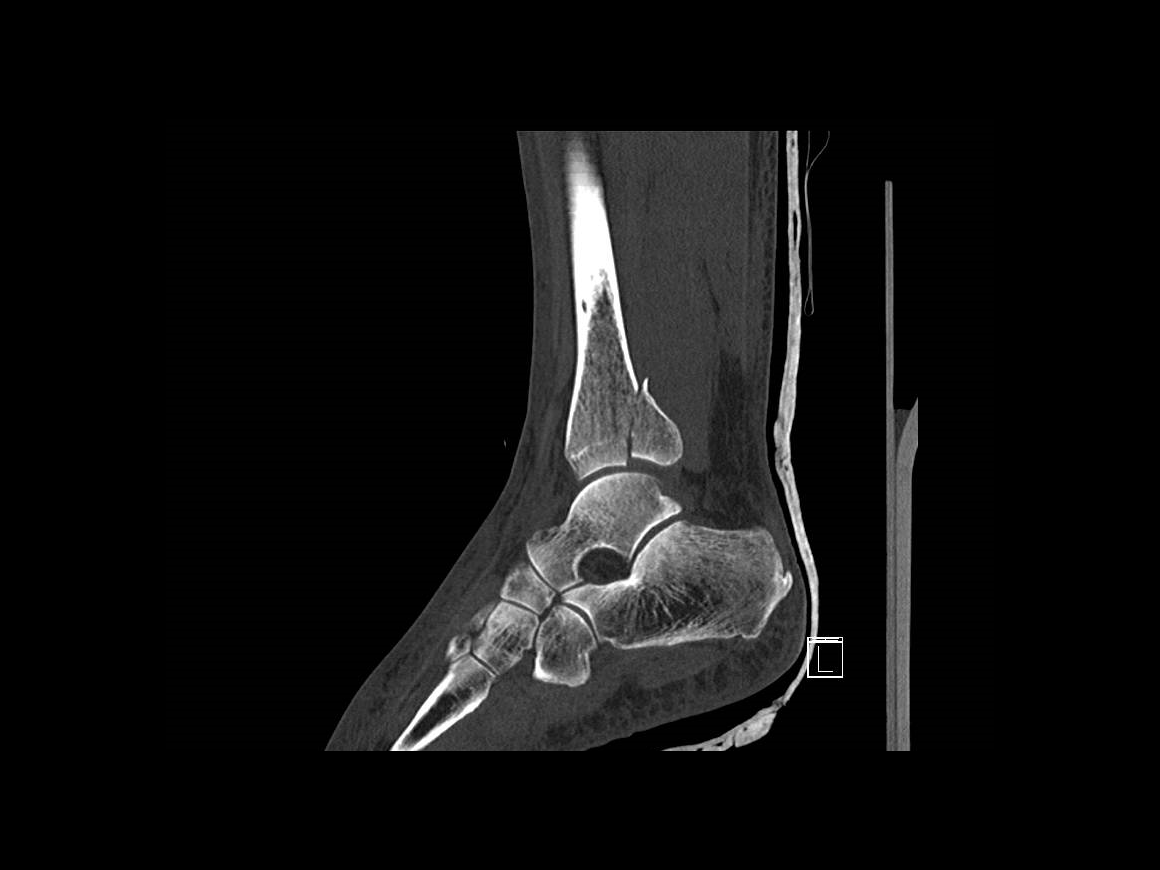
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Ankle fracture: Posterior malleolar fixation using a posteromedial approach surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle fracture: Posterior malleolar fixation using a posteromedial approach surgical procedure.
Ankle fractures with involvement of the posterior malleolus are recognised as having a poorer outcome however the management and indications for fixation of the posterior malleolus remain poorly defined. Fixation of posterior malleolar fractures was first described by Lounsbury and Metz in 1922 who used an extensile medial approach to fix large posterior fragments with a bone peg. Traditional teaching subsequently advocated fixation of posterior malleolar fragments based on their size when assessed on a lateral radiograph with fixation being recommended for fragments representing either a quarter or a third of the articular surface.
Recently there has been a paradigm shift in treatment of posterior malleolar fractures as it has become recognised that the size of the posterior malleolar fragment alone is not the only predictor of outcome. Factors such as articular congruence, posterior stability of the joint and ligamentous stability of the ankle are also important determinants of outcome.
There are a number of classifications describing the posterior malleolus however most are a development of that described by Haraguchi, dividing them into three types based on the appearance on axial CT. The Haraguchi type 1 injury is a large posterolateral fragment involving the posterior syndesmotic ligament, a Haraguchi type 2 posterior malleolar fracture extends medially and often has two distinct fragments: posterior and posteromedial with the posteromedial fragment extending to involve the posterior colliculus of the medial malleolus and thus the attachment of the deep deltoid can be rendered unstable by this fragment. A type 3 injury is a sleeve avulsion of the posterior syndesmotic ligament, this pattern is usually not amenable to fixation and syndesmotic stability is achieved indirectly with syndesmotic screws or equivalent.
Surgical fixation of the posterior malleolus can be performed by a number of approaches. Traditionally it was achieved with the patient in a supine position, indirect reduction of the fragment and fixation with screws inserted from anterior to posterior to capture the fragment. It is increasingly recognised however that direct fixation of the fragment via a posterior approach is biomechanically superior.
The most common posterior approach is the posterolateral with an interval between the peronei and flexor hallucis longus, this affords good visualisation of the posterolateral fragment (Haraguchi 1) and also enables fixation of the fibula fracture via the same incision in most cases. This approach however does not allow fixation of posterior malleolar fractures with medial extension and thus in my hands Haraguchi type 2 fractures are often better fixed via a posteromedial approach. This can be performed in a variety of ways, often via the bed of tibialis posterior. In this technique I describe an approach which allows fixation the posteromedial and posterolateral fragments via the same incision utilising windows either side of the posterior neurovascular bundle.
OrthOracle readers will also find the following associated instructional techniques of interest:
Posterior ankle decompression- Open technique
Tarsal tunnel decompression (for tarsal tunnel syndrome)
Ankle fracture: Medial malleolar fixation with ASNIS screws
Ankle fracture : Fibula pro-tibia fixation technique with Stryker Variax plate.
Ankle fracture: Lateral malleolar fixation using Acumed Fibula Rod System
Author: Paul Fenton, FRCS (Tr & Orth)
Institution: The Queen Elisabeth Hospital, Birmingham, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















