Anterior Cervical Decompression and Fusion using Globus coalition MIS cage
Overview
Subscribe to get full access to this operation and the extensive Spine Surgery Atlas.
Learn the Anterior Cervical Decompression and Fusion using Globus coalition MIS cage surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Anterior Cervical Decompression and Fusion using Globus coalition MIS cage surgical procedure.
Degenerative cervical myelopathy (DCM) is the commonest cause for spinal cord impairment in adults. This term includes cervical spondylotic myelopathy, ossification of the posterior longitudinal ligament, ossification of the ligamentum flavum and degenerative disc disease. Progressive compression of the spinal cord leads to functional impairment. The burden of disease in the community is likely to rise as a result of the ageing population.
The pathophysiology is spinal cord compression from both static factors and dynamic factors, as a result of age-related changes in the cervical spine. There is resultant ischaemia, inflammation and apoptosis of glial cells.
Patients present with progressive neurological deficits affecting the upper and lower limbs, most commonly deterioration in manual dexterity and gait disturbance. The natural history of this condition is varied. Some patients have long periods of stable symptoms, whereas others experience rapid functional declines.
DCM can be classified as mild, moderate or severe according to the modified Japanese Orthopaedic Association score. This system has 4 domains; upper extremity motor score (5), lower extremity motor score (5), upper extremity sensory score (3) and urinary function score (3). A cumulative score of 0-11 indicates severe DCM, 12-14 indicates moderate DCM and 15-17 indicates mild DCM.
Current guidelines recommend surgical treatment for patients with moderate or severe myelopathy. Patients with mild myelopathy should be offered surgical treatment or a supervised trial of structured rehabilitation, with the option of surgery if conservative management fails.
The aims of surgical treatment of DCM are to achieve a robust decompression of the spinal cord, and leave a stable vertebral column.
Surgery can be approached from the front of the neck or the back of the neck. There are several factors to take into account when deciding the surgical approach, which are detailed in the indications section.
The anterior approach to the cervical spine is an elegant surgical approach that takes advantage of fascial planes and visceral and vascular mobility to provide fairly atraumatic direct access to the anterior column of the spine. This approach can be used to address single or multi-level disease of a range of pathologies including degenerative disease, tumour, trauma and infection.
The most common indication is degenerative disease. Both the spinal cord and the nerve root can be decompressed, meaning this is the surgical treatment for cervical myelopathy and cervical radiculopathies.
Following anterior cervical discectomy the segment is fixed and over time a bony fusion takes place.
There are a range of fixation strategies available including stand-alone cages, cage and plate and more modern systems that comprise cage and integrated plates. The addition of a plate reduces torsional and compressive forces and reduces the risk of cage subsidence. Fusion rates increase with the addition of instrumentation, going from 60% with no cage, to 92% with a cage and 95% with a cage and plate. In practice some instrumentation is always used except in cases of cervical discitis when the surgeon may opt to avoid any implants. The addition of instrumentation however increases operating time and a plate can be associated with other complications including dysphagia, screw misplacement and plate migration. A plate can can also complicate future surgical treatment of adjacent level disease by limiting the fixation options available.
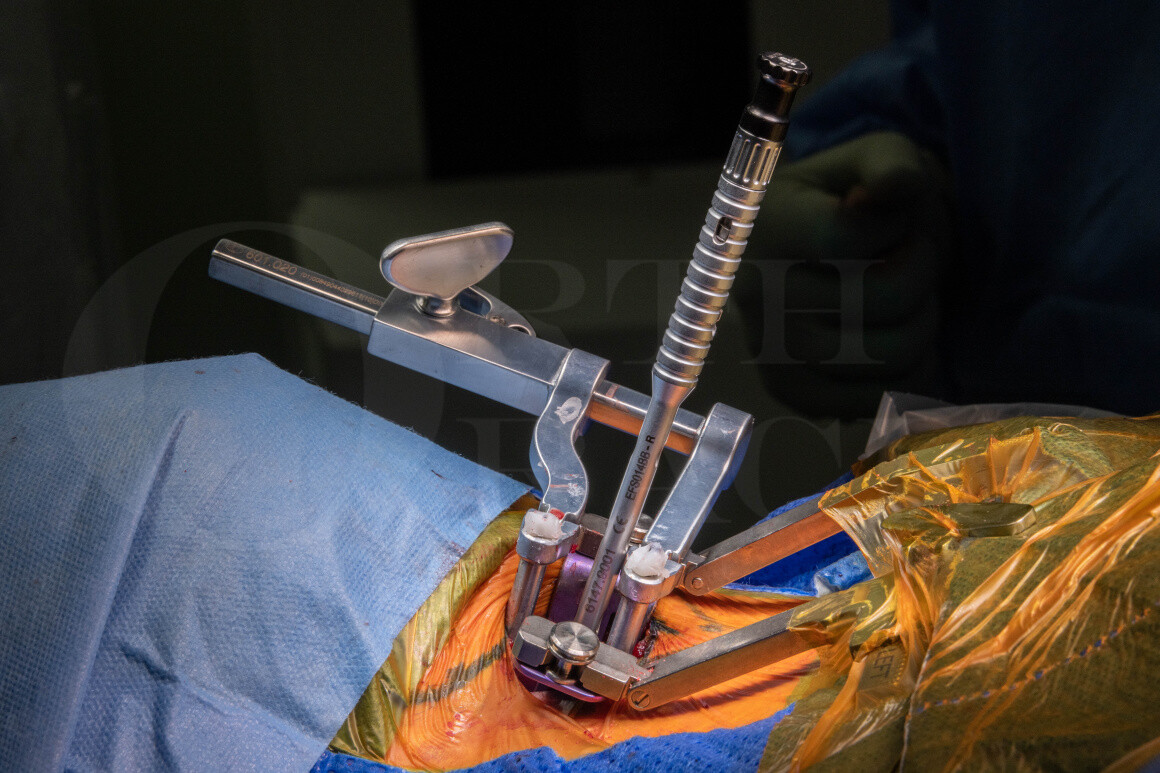
In this case I have chosen the Globus MIS coalition cage with screws. The unique selling points with this implant are the integrated interbody cage and plate, held in place by screws. This provides added biomechanical strength and avoids the risks of plate fixation.
OrthOracle readers will also find the following instructional techniques of interest:
Cervical microdiscectomy via posterior foraminotomy
Cervical spine decompression: Posterior approach (Degenerative cervical myelopathy).
Cervical laminectomy and resection of spinal cord tumour
Anterior Cervical Discectomy and Fusion using the DePuy Zero-P VA cage
Cervical Laminoplasty for treatment of Cervical spondylotic myelopathy
Author: Mark Nowell FRCS
Institution: Southmead Hospital, Bristol, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















