Patello-femoral replacement: Avon implant (Stryker)
Overview
Subscribe to get full access to this operation and the extensive Knee Surgery Atlas.
Learn the Patello-femoral replacement: Avon implant (Stryker) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Patello-femoral replacement: Avon implant (Stryker) surgical procedure.
Partial knee replacement is an alternative to total knee arthroplasty when there is a localized pattern of arthritis effecting a single compartment of the knee. There are three well-documented patterns of knee arthritis:
- Medial – this is an anteromedial pattern with a preserved posteromedial ‘shelf’ of medial plateau which maintains the functional length of the Medial Collateral Ligament.
- Lateral – this is more posterocentral in the lateral compartment giving a flexion pain and instability
- Patellofemoral – this is often associated with either patella alta (the patella situated proximal relative to the trochlea) or trochlea dysplasia (where there is an abnormal development of the PFJ with lateral dominance and a shallow or even domed trochlea groove)
There has been considerable concern over partial knee replacement as the revision rates for these procedures is recorded as being higher than that for total knee arthroplasty on multiple registries. Consequently the longevity of partial knee replacement is lower than total knee arthroplasty in large data-sets. However there are also distinct advantages both to patients and when regarding the broader health care economics of the procedure, as is now evident from the published results of prospective randomized controlled trials of total versus partial (unicompartmental and patellofemoral) knee arthroplasty. The complication rates and mortality rates are certainly lower when comparing the results of partial to total knee arthroplasty.
The most notable of papers that readers should be familiar with are:
The clinical and cost-effectiveness of total versus partial knee replacement in patients with medial compartment osteoarthritis (TOPKAT): 5-year outcomes of a randomised controlled trial. Beard DJ et al. Published:July 17, 2019 DOI:https://doi.org/10.1016/S0140-6736(19)31281-4
Patellofemoral Arthroplasty Results in Better Range of Movement and Early Patient-reported Outcomes Than TKA. Odgaard A, Madsen F, Kristensen PW, Kappel A, Fabrin J. Clin Orthop Relat Res. 2018 Jan;476(1):87-100. This paper shows a better functional outcome for PFJ than TKA up to 9 months in may patient reported domains, but by 2 years the only difference is better flexion by 10 degrees in the PFJ group compared to the TKA.
Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients: a study of data from the National Joint Registry for England and Wales. Liddle AD, Judge A, Pandit H, Murray DW. Lancet. 2014 Oct 18;384(9952):1437-45
45-day mortality after 467,779 knee replacements for osteoarthritis from the National Joint Registry for England and Wales: an observational study. Hunt LP, Ben-Shlomo Y, Clark EM, Dieppe P, Judge A, MacGregor AJ, Tobias JH, Vernon K, Blom AW; National Joint Registry for England and Wales. Lancet. 2014 Oct 18;384(9952):1429-36.
How long does a knee replacement last? A systematic review and meta-analysis of case series and national registry reports with more than 15 years of follow-up.Evans JT, Walker RW, Evans JP, Blom AW, Sayers A, Whitehouse MR.Lancet. 2019 Feb 16;393(10172):655-663. doi: 10.1016/S0140-6736(18)32531-5. Epub 2019 Feb 14. Erratum in: Lancet. 2019 Feb 20
The Odgaard paper is the most relevant for this operation technique section, but whilst there are significant benefits for patients with isolated patellofemoral joint OA to undergo patellofemoral arthroplasty it is important to discuss disease progression and possible future revision in order to reach a balanced and mutual decision on which operation is best for each individual patient.
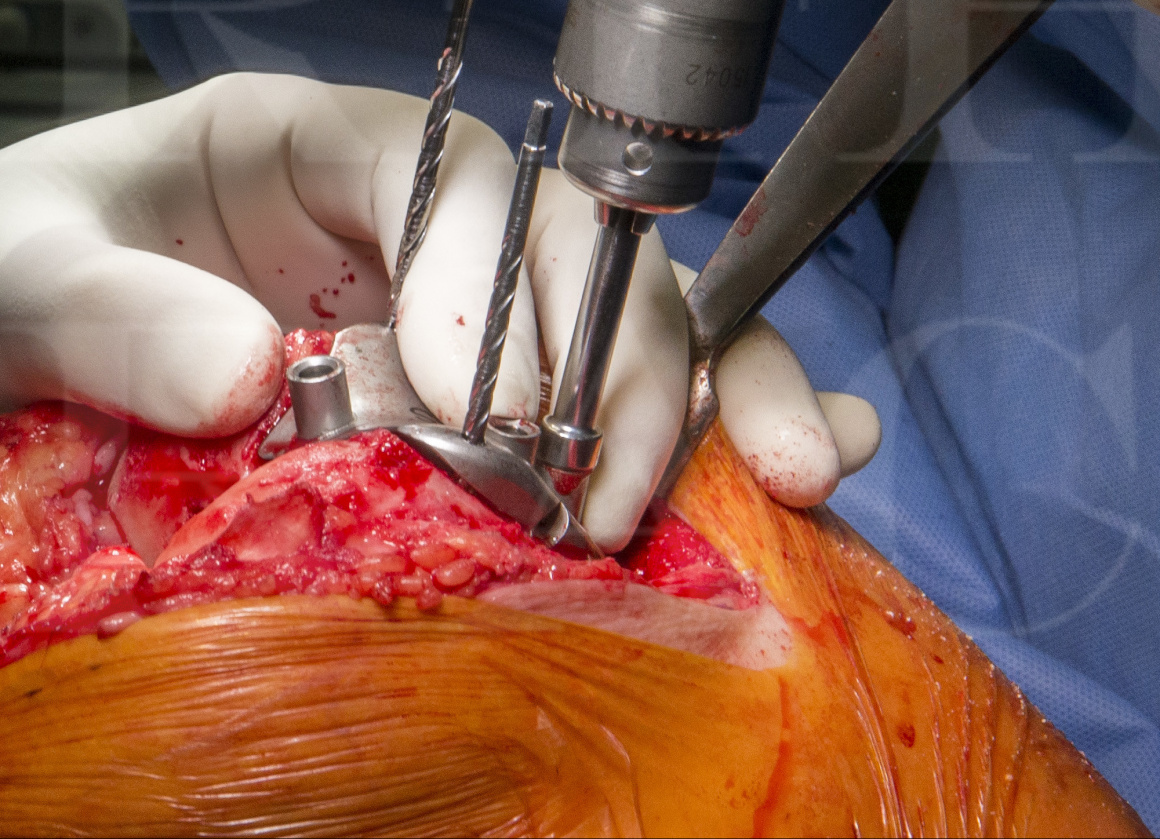
The Avon patellofemoral joint arthroplasty is a non-sided onlay design which resects the degenerative anterior trochlea and diseased chondral surface of the patella. There is no size constraint to match patella size to trochlea component, in order to achieve correct sizing of each component independently.
Author: James Murray FRCS (Tr & Orth)
Institution: The Avon Orthopaedic Centre, Southmead Hospital, Bristol, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















