Calcaneal fracture: Primary arthroscopic subtalar fusion
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Calcaneal fracture: Primary arthroscopic subtalar fusion surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Calcaneal fracture: Primary arthroscopic subtalar fusion surgical procedure.
The optimum management of calcaneal fractures remains elusive. They are often severe injuries, causing long-term disability. The evidence for surgical reconstruction and fixation is certainly growing but there is yet to be a definitive benefit with surgery for the majority of fractures.
The Sanders classification is most commonly used and is prognostic – the classification depends on the injury to the posterior facet of the subtalar joint. It classifies according to the number of displaced articular fragments on the widest Coronal CT slice: Displaced two part fracture of the posterior facet (Type 2), three part (Type 3) or more severely comminuted (Type 4). (There is a sub-classification (A,B,C) which depends on the medial / lateral position of the fracture – it is not prognostic and rarely used).
1. Sanders R, Fortin P, DiPasquale T, Walling A. Operative treatment in 120 displaced intraarticular calcaneal fractures. Results using a prognostic computed tomography scan classification. Clin Orthop Relat Res. 1993
More recently, HEFT trial in the UK reported on the outcomes of surgery vs conservative treatment. The paper had some severe flaws and some very misleading conclusions, as the majority of severe fractures were excluded from the study! As such, it really only compared minimally displaced fractures. The review and critique and of this paper by Chris Pearce in the BJJ is well worth reading.
2. Pearce CJ, Wong KL, Calder JD. Calcaneal fractures: selection bias is key. Bone Joint J. 2015
The traditional surgical approach is based on a long L-shaped lateral incision, with exposure of the whole of the lateral side of the calcaneum and the subtalar joint. This allowed removal of the lateral joint fragments, to expose the medial joint surfaces with reconstruction starting on the medial side, building up laterally to achieve as anatomical a reduction as possible. The skin exposure is based on the blood supply from the lateral calcaneal artery, a branch of the peroneal artery. Despite this, the wound complication rates are high – in the region of 25% or more, with approximately an 8-10% risk of deep infection. This continues to be a concern and strong reason to treat cases non-operatively.
More recently, “minimally invasive” approaches have become popular, especially the sinus tarsi approach. This is a much smaller incision, based at the level of the subtalar joint. There is much less soft-tissue trauma but with a limited exposure of the joint surfaces. The wound complications are still significant at 10-15%.
Arthroscopic techniques have also been reported on – there are few published reports but there is a significant reduction in wound complications and infection rates. The technique is challenging and there are more papers being published on it, with consistently improved complication rates – I have been using this technique since 2007 for the majority of calcaneal fractures (Type 2 & Type 3) and now use arthroscopy to manage the more severe fractures with primary arthroscopic fusion.
3. Pastides PS, Milnes L, Rosenfeld PF. Percutaneous Arthroscopic Calcaneal Osteosynthesis: A Minimally Invasive Technique for Displaced Intra-Articular Calcaneal Fractures. J Foot Ankle Surg. 2015
Despite these advances, the functional outcomes after calcaneal fixation are still mediocre with joint stiffness and pain still significant. This presents as continued pain over the lateral hindfoot in the subfibular region with stiffness and rigidity (although the stiffness is rarely disabling on its own). Certainly, it is common to need steroid injections into the subtalar joint for pain relief and in more severe cases, further surgery to fuse the subtalar joint. Later fusion is more common with increased fracture severity (20% in Type 2 and 45% in Type 3 fractures.)
4. Sanders R, Vaupel ZM, Erdogan M, Downes K. Operative treatment of displaced intraarticular calcaneal fractures: long-term (10-20 Years) results in 108 fractures using a prognostic CT classification. J Orthop Trauma. 2014
The consensus view at present is that displaced 2-part fractures should do well with reduction and internal fixation, with reasonable long term prospects. The outcomes following displaced 3-part fractures are still poor and there is little evidence to show that they are much better than conservative management. For more severely comminuted fractures, the evidence is against open reduction, with primary fusion of the subtalar joint being recommended – The goal here of course is to stiffen the joint permanently but to minimise any long-term disability from arthritis.
5. Buckley R, Tough S, McCormack R, Pate G, Leighton R, Petrie D, Galpin R. Operative compared with nonoperative treatment of displaced intra-articular calcaneal fractures: a prospective, randomized, controlled multicenter trial. J Bone Joint Surg Am. 2002
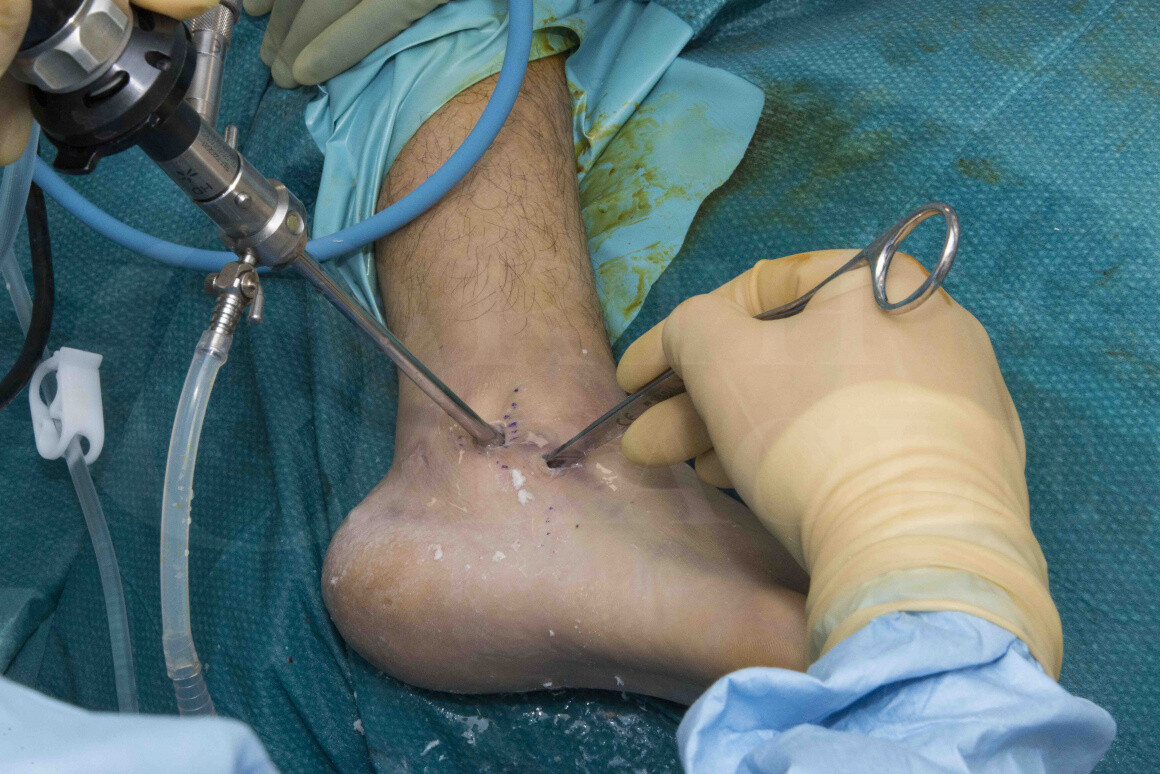
Having managed calcaneal fractures arthroscopically for many years now, I have been using primary arthroscopic arthrodesis for the more complex 3 or 4 part fractures. In this case, the patient has a displaced articular fracture, affecting the posterior subtalar joint. There is joint depression with comminution and unusually impaction too – it is not a classical 3 or 4 part fracture but is definitely worse than 2 part. The patient’s goal is to continue playing amateur football and as such, I advised a primary arthroscopic subtalar fusion as the best way to achieve this.
OrthOracle readers will also find the following associated operative techniques of interest:
Calcaneal fracture: fixation with extended lateral approach and ZimmerBiomet ALPS plate
Calcaneal fracture: Percutaneous fixation of Tongue-type fracture.
Calcaneal fracture fixation: Extended lateral approach and locking plate fixation
Calcaneal fracture fixation : Internal fixation of sustentaculum tali fracture (Acutrak screws)
Triple fusion: For calcaneal fracture malunion
Author: Peter Rosenfeld FRCS(Tr & Orth)
Institution: St Marys Hospital & The Fortius clinic, London, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















