Hallux Rigidus: First MTP Fusion using Coughlin reamer and Orthosolutions Cannulated 4mm screws
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Hallux Rigidus: First MTP Fusion using Coughlin reamer and Orthosolutions Cannulated 4mm screws surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Hallux Rigidus: First MTP Fusion using Coughlin reamer and Orthosolutions Cannulated 4mm screws surgical procedure.
A 1st MTP (metatarsophalangeal ) joint fusion is a highly versatile operation both in terms of the conditions which can be treated as well as in terms of the function possible after successful fusion.
A union rate of 90% plus is recorded in most series using current techniques. Success defined in terms of patient satisfaction rates though can be slightly lower than those of radiographic union of the fusion .
The keys to operative success are careful joint preparation, positioning and appropriate fixation.
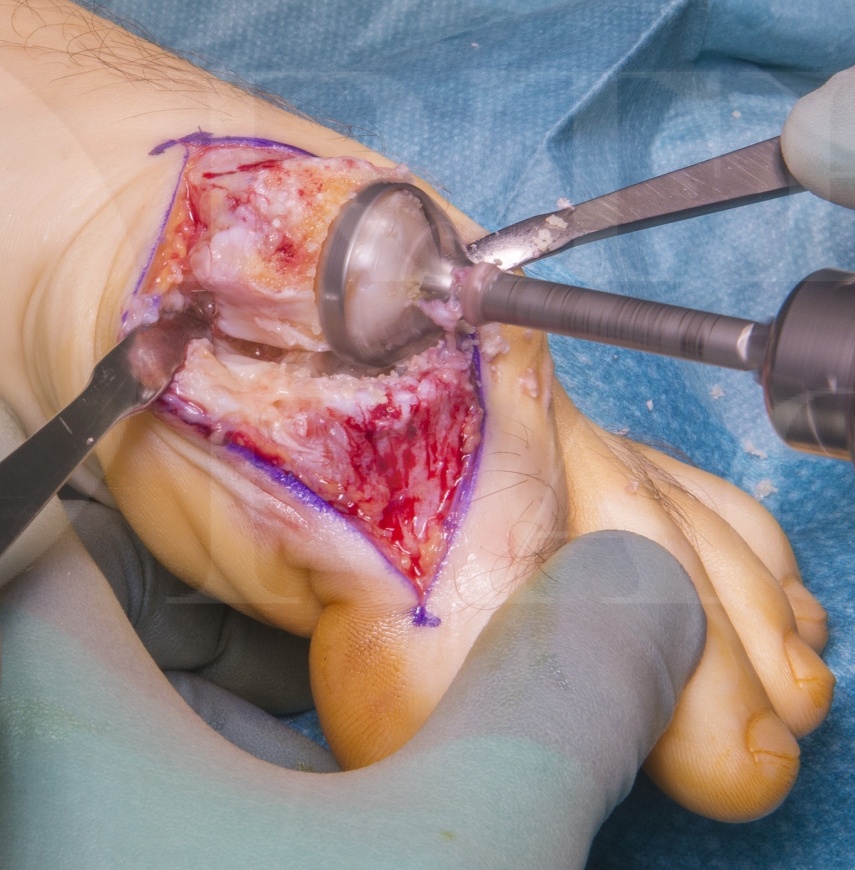
Successful union of requires adequate preparation of the articular surfaces to expose subchondral bone, and rigid internal fixation. The technique described uses reciprocal dome shaped reamers to provide a congruent ‘ball and socket’ interface for fusion, this allows more versatility in aligning the toe optimally than flat cuts, provides a large surface area for fusion, and can be used to correct concomitant hallux interphalangeus.
There are various ways of fixing the fusion, most commonly a single axial compressive screw combined with a dorsal neutralising or compression plate . The technique detailed in this operation is a “crossed-screws” technique which differs only in the final mode of fixation.
Author : Mr Nick Cullen FRCS (Tr & Orth)
Institution :The Royal National Orthopaedic Hospital ,Stanmore ,UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















