L4-S1 navigated transforaminal lumbar interbody fusion and decompression using Medtronic Solera and Artic-L
Overview
Subscribe to get full access to this operation and the extensive Spine Surgery Atlas.
Learn the L4-S1 navigated transforaminal lumbar interbody fusion and decompression using Medtronic Solera and Artic-L surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the L4-S1 navigated transforaminal lumbar interbody fusion and decompression using Medtronic Solera and Artic-L surgical procedure.
Lumbar spinal stenosis is a very common condition affecting up to up to 47% of adults over 60 years old, although only around 9% may be symptomatic. Symptoms often come on with standing or walking and improve with leaning forwards or sitting down. In some instances, patients may also experience a radiculopathy while at rest.
Spinal stenosis can occur at any level of the spine. It is most commonly caused by facet joint hypertrophy, ligamentum flavum hypertrophy, and degenerative broad disc bulges. Since the lumbar spine and cervical spine move more than the thoracic spine, stenotic changes are more common in these mobile sections of the spine. More forces go through the lumbar spine which means stenotic changes are most common in this area.
Spinal stenosis can effect the central canal and lateral recesses but may also cause foraminal stenosis. It can also be associated with spondylolisthesis, retrolisthesis, and lateral listhesis as well as any spinal deformity. There is also a subgroup of patients who have congenital stenosis that predisposes them to becoming symptomatic if they develop degenerative changes later in life.
The condition often presents insidiously with spinal claudication. This manifests itself as paraesthesia or aching, progressing to pain and weakness. Patients typically have spinal claudication effecting both lower limbs but it can present unilaterally. The pain often starts when patients have been standing in one position for more than a few minutes, or if they walk for more than 5-10 minutes. Patients will often complain symptoms are worse if they have to walk slowly around shops. However, leaning forward on a stick, frame, or shopping trolley often alleviate their symptoms since flexion makes the lumbar spinal canal wider. Patients also describe that they need to sit down or lean forwards to allow their symptoms to resolve.
The vast majority of patients can be managed non-operatively and should be encouraged to stay as active as possible, with modification of activities that bring on their symptoms. However, for those who have exhausted non-operative measures, surgery may be beneficial.
Surgical management options available include lumbar decompression or fusion with decompression. In some patients, decompression procedure alone may not achieve satisfactory decompression of the nerves to improve symptoms. In this situation, the surgeon needs to work out if excision of the facet joints will achieve decompression. If the facet joints are excised, instrumentation is required to achieve stability of that spinal segment.
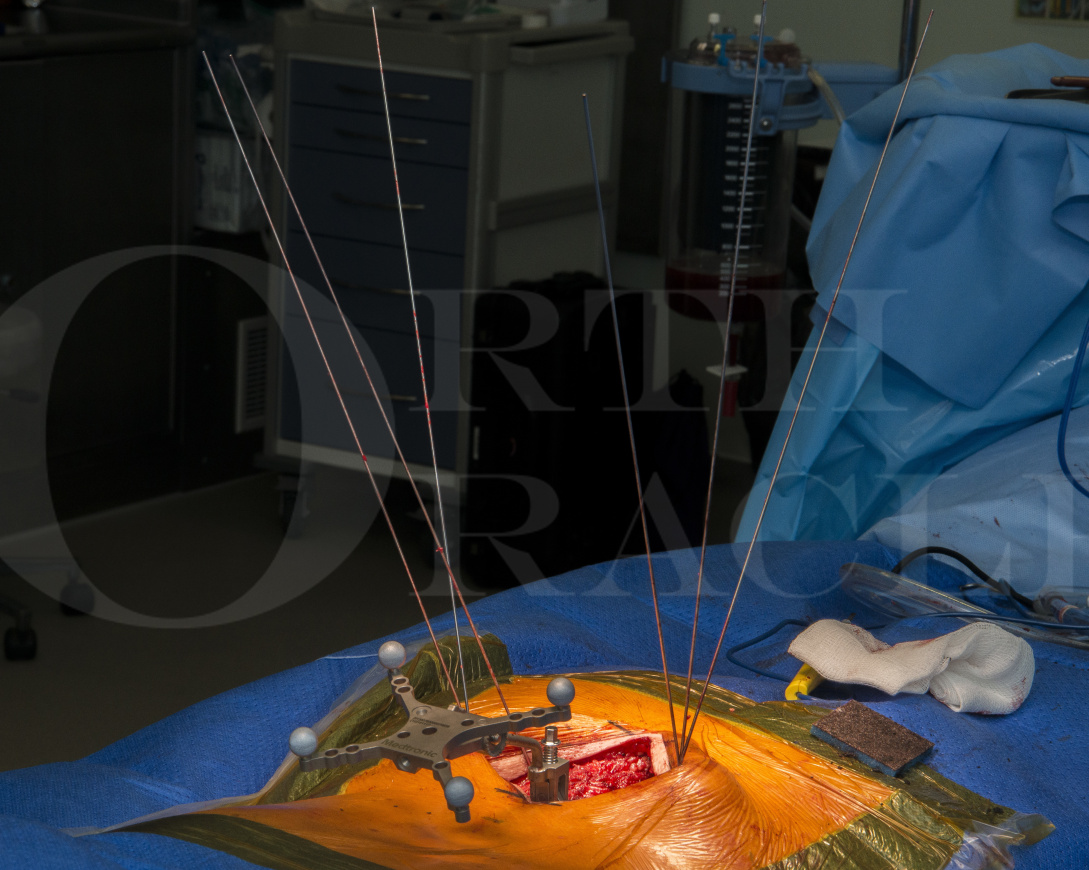
In this procedure, I have used multiaxial screws which can be navigated; for lumbar degenerative work, it is uncommon to require fixed angle screw heads. The interbody cage has been designed to allow control of the cage at all stages during insertion which makes it possible to change the position of the cage, if required. I use a transforaminal interbody (TLIF) cage since this can be positioned anteriorly in the disc space in order to create lordosis across the segment, compared to a posterior interbody (PLIF) cage which are often less lordotic and allow less compression posteriorly.
Author: Mr Stephen Morris FRCS (Tr & Orth).
Institution: The Avon Orthopaedic Centre, Southmead Hospital, Bristol, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















