Lumbar microdiscectomy for cauda equina syndrome
Overview
Subscribe to get full access to this operation and the extensive Spine Surgery Atlas.
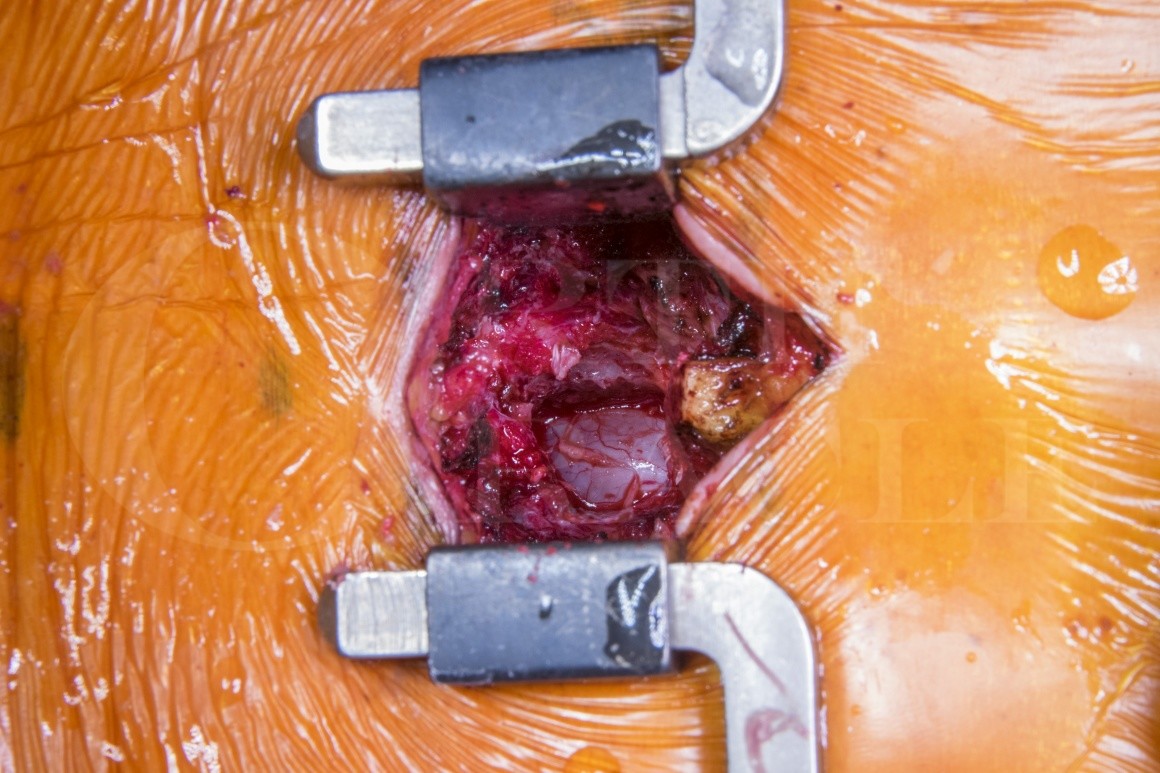
Learn the Lumbar microdiscectomy for cauda equina syndrome surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Lumbar microdiscectomy for cauda equina syndrome surgical procedure.
Lumbar disc prolapse is a common condition. Cauda equina syndrome is a rare complication of disc prolapse and occurs in around 1.8 per million people. It may present with back pain and/or sciatic pain, bladder or bowel dysfunction, perineal or saddle anaesthesia, and unilateral or bilateral lower limb radiculopathy. It can affect patients of any age but is more common in patients with disc degeneration
It can be divided into CES with retention (CES-R) where there is painless urinary retention, or CES incomplete (CES-I) where there is alteration of normal bladder and bowel function. Both conditions should be investigated and treated as an emergency to prevent long-term sequelae and disability with persistent bladder and bowel dysfunction. It is a different condition to those uncommon elderly patients who have critical spinal stenosis and may have intermittent perineal numbness which comes on at the same time as lower limb claudication symptoms and resolves with sitting.
There has been debate over the years of the critical time to surgery, with this varying from 6 hrs up to 48hrs. The British Association of Spine Surgeons (BASS) and the Society of British Neurological Surgeons (SBNS) published recommendations in Dec 2018 which suggest operating at the earliest safe opportunity. This depends on local expertise, the available resources, and the duration of symptoms.
This feature discusses the features of cauda equina syndrome and how to manage this. It is an important aspect of spinal pathology to be familiar with if you are involved with any aspect of emergency care, spinal or orthopaedic patients.
Author: Mr Stephen Morris FRCS (Tr & Orth)
Institution: The Avon Orthopaedic Centre, Southmead Hospital, Bristol, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















