MCP joint fusion of thumb (tension band wiring technique)
Overview
Subscribe to get full access to this operation and the extensive Upper Limb & Hand Surgery Atlas.
Learn the MCP joint fusion of thumb (tension band wiring technique) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the MCP joint fusion of thumb (tension band wiring technique) surgical procedure.
The thumb consists of three joints; the carpometacarpal joint(basal joint), metacarpophalangeal joint and the interphalangeal joint. Whilst the basal joint is a saddle joint which allows movements in multiple planes, the other two are hinge joints which allow flexion and extension. The metacarpophalangeal (MCP) joint provides stability for pinch grip. The range of movements of this joint do vary between individuals and in some people the joint has very limited natural flexion.
This joint can be effected be trauma and degenerative conditions. One common traumatic pathology which can lead to degenerative joint change here is injury to the ulnar collateral ligament which in the acute setting is called ‘Skier’s thumb’. If diagnosed in time this ligament can be repaired. Chronic laxity of the ligament due to repeated stressing is known by the eponym ‘Game-keeper’s thumb.’
The common degenerative pathologies effecting the MCP joint are osteoarthritis and rheumatoid arthritis. In osteoarthritis the joint develops inflammation and stiffness and commonly remains fairly well aligned. In contradistinction with rheumatoid arthritis complex deformity ranging from a Boutonniere to a Swan neck deformity can be associated with the degenerate joint.
The most definitive end stage surgical treatment for pathological conditions that result in severe MCP joint degenerative change (with or without deformity) is fusion. High levels of function can be expected as long as the remaining joints are functioning well. Replacements, though a technical possibility, have a tendency to early failure and sub-optimal function due to the high functional requirements of the thumb MCP joint.
There are several common methods for fixing an MCP joint fusion including K-wires, tension band-wiring, screw fixation alone and plate and screw fixation. Each of the techniques have their advantages and disadvantages.
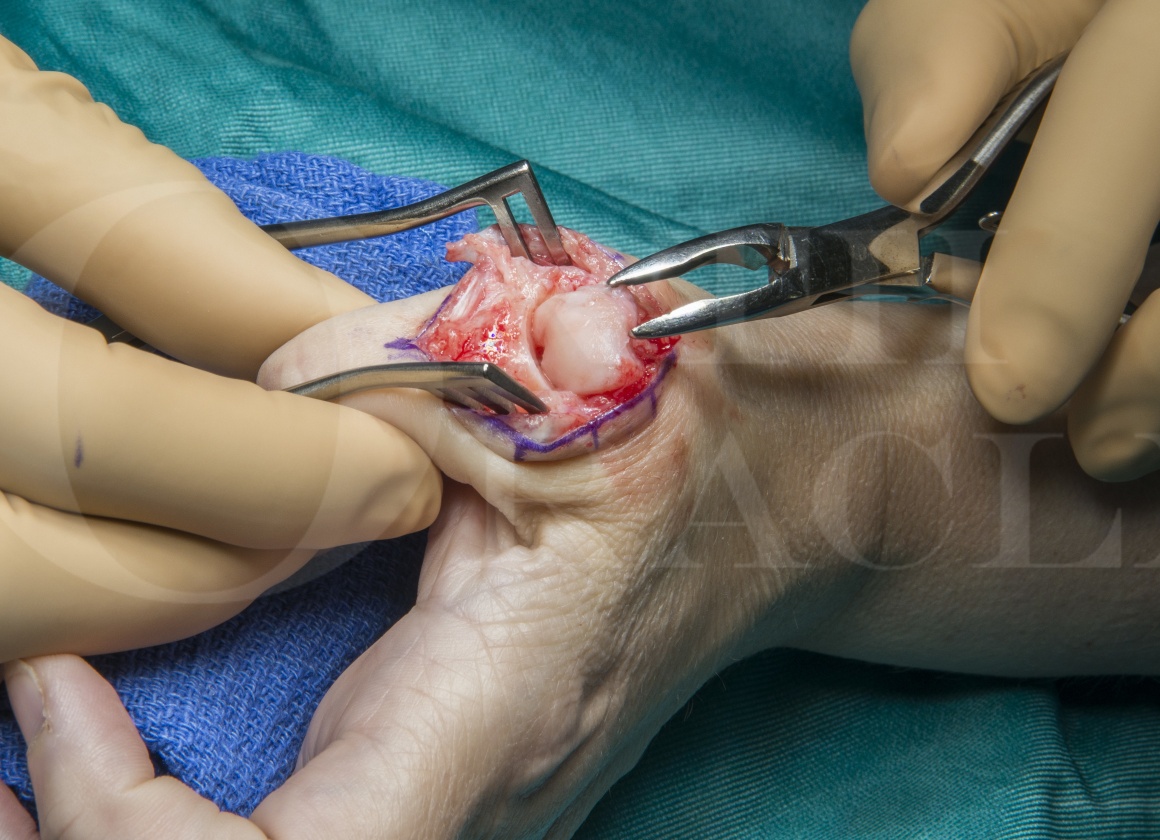
The case below illustrates the use of tension band wiring for performing a fusion of the MCP joint in a patient who has osteoarthritis and ulnar collateral laxity of the joint.
Author: Mr Rajive Jose FRCS
Institution : The Queen Elizabeth Hospital ,Birmingham ,UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















