Acromioclavicular joint: Open excision (Mumford procedure)
Overview
Subscribe to get full access to this operation and the extensive Shoulder & Elbow Surgery Atlas.
Learn the Acromioclavicular joint: Open excision (Mumford procedure) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Acromioclavicular joint: Open excision (Mumford procedure) surgical procedure.
This is a useful technique to be able to offer to patients with a acromioclavicular joint pain secondary to degenerative change. Isolated acromioclavicular joint pain is quite common and can vary in severity, from being either a minor inconvenience to interfering significantly with work, sport and leisure activities and in particular sleep.
The clavicle is one of the last bones to fully ossify in the human skeleton and almost as soon as it has done so there is propensity for it to degenerate at either the medial sternoclavicular joint or more commonly at the lateral acromioclavicular joint. The onset of pain in the acromioclavicular joint can be insidious or maybe as a result of minor trauma such as a grade 1 or a grade 2 sprain, which comes about as a fall directly on to the point of the shoulder or a direct blow to the acromioclavicular joint.
It has been documented that approximately 30% of the population have an intra-articular disc of soft tissue similar to a knee meniscal cartilage within the acromioclavicular joint. If this were to be damaged, then that can also be a cause of persistent pain and disability.
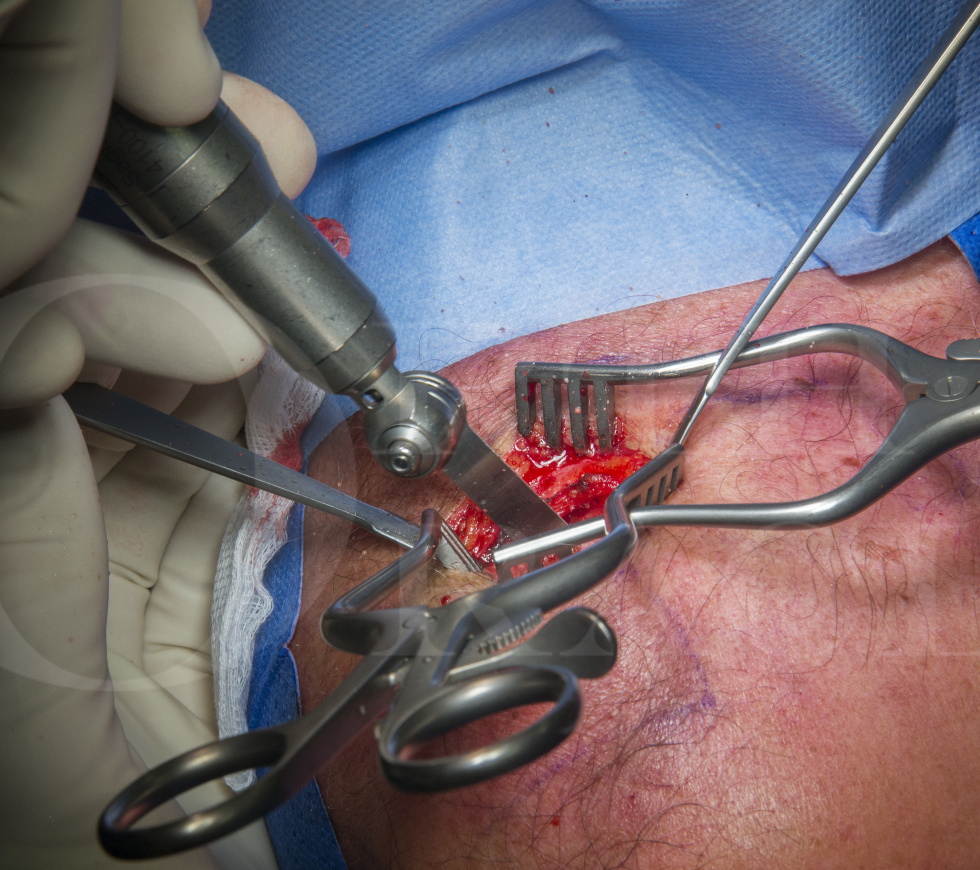
Once a diagnosis of acromioclavicular joint pain has been established then simple conservative measures should be recommended in the first instance. If non-operative measures have been exhausted and the patient has persistent pain, then consideration should be given to excision arthroplasty of the acromioclavicular joint with removal of the joint contents and resection of the distal clavicle articular facet. This is also known as the Mumford procedure after an early description published in 1941. The cavity then fills with scar tissue and generally the patient’s symptoms are greatly improved quite quickly. The open technique described here is relatively quick, straightforward and successful.
Author: Mr Mark Crowther FRCS (Tr & Orth)
Institution: The Avon Orthopaedic centre, Southmead Hospital, Bristol, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















