Flexor tendon repair: Reattachment of Flexor digitorum profundus using mini-mitek bone anchor
Overview
Subscribe to get full access to this operation and the extensive Upper Limb & Hand Surgery Atlas.
Learn the Flexor tendon repair: Reattachment of Flexor digitorum profundus using mini-mitek bone anchor surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Flexor tendon repair: Reattachment of Flexor digitorum profundus using mini-mitek bone anchor surgical procedure.
Avulsion injuries of flexor tendons injuries occur usually as part of contact sports. Flexor Digitorum Profundus of the ring finger is the most commonly effected one. These are eponymously sometimes called “Jersey finger” as often these injuries occur when the finger is caught in a player’s jersey during contact. The tendon may be avulsed cleanly from the bone or may become detached with a piece of the phalangeal bone. These injuries have been classified by Leddy and Packer into three types:
Type 1. No bony fragment and the tendon retracts into A1 pulley area.
Type 2: A small bony fragment and the tendon retracts into the A3 pulley area as the bone fragment is caught in the chiasma of the FDS slips
Type 3: A large bony fragment resulting in no significant retraction as the fragment cannot pass through the sheath.
A Type 4 has later been added which equates to a Type 3 where the bone has then detached from the tendon which retracts into the A1 pulley.
Patients often present late after the event. The nature of an adrenaline charged contact sport means these injuries are often ignored at the time and it is only when the swelling and pain ensues that the loss of movements of the finger is noted.
On examination there is swelling and bruising around the finger when they present early. Patients are unable to flex the DIP joint actively.
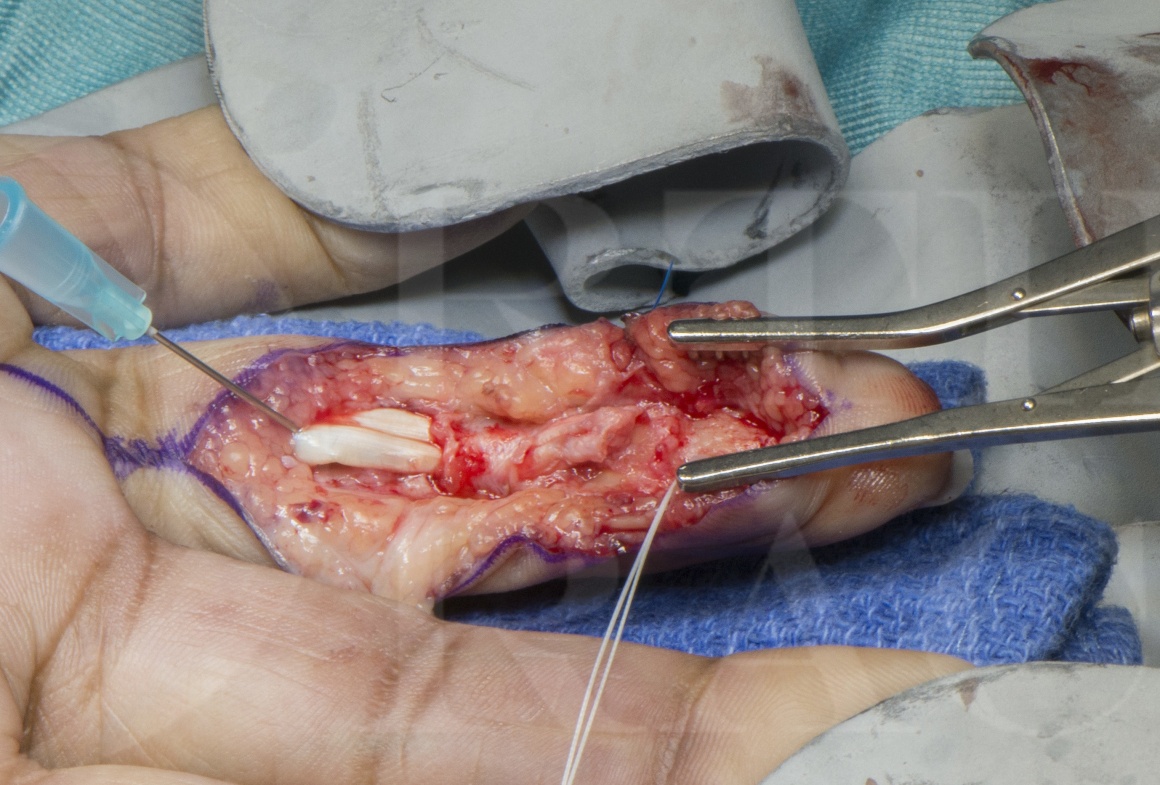
The treatment depends on the type of injury. If the tendons has been avulsed off without a bony fragment, the finger is explored through a zig-zag incision and the tendon end retrieved. It is reattached using a variety of methods. These include drilling into bone and passing a non-absorbable suture from the tendon into the bone, passing the suture across the nail and tying it over a button or a sponge, or reattaching it using a bony anchor. If there is a substantial bone fragment, it has to reattached using screws or a small plate and screws. If the bony fragment is small it can be excised and tendon reattached .
If presenting later than two weeks the tendon may shorten especially in Type 3 injuries. If during the operation the tendon is found tight and even on stretching does not reach the distal phalanx and decision has to be made as to whether a primary tendon grafting should be considered or to do a DIP joint fusion at a later date. Undue flexion of the finger from a very tight repair can result in PIP and DIP joint contractures which may not correctable later.
In these cases patients should be counselled about the merits and risks of tendon reconstruction. If the lack of DIP joint flexion is not a significant problem, it is better to leave it alone. If patient’s functional demands require the DIP joint to be in flexion, then a DIP joint fusion is a simpler and effective alternative to tendon reconstruction.
Author: Mr Rajive Jose FRCS.
Institution: The Queen Elizabeth Hospital, Birmingham, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















