Sacro-iliac joint fusion, minimally invasive technique with iFuse implant
Overview
Subscribe to get full access to this operation and the extensive Spine Surgery Atlas.
Learn the Sacro-iliac joint fusion, minimally invasive technique with iFuse implant surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Sacro-iliac joint fusion, minimally invasive technique with iFuse implant surgical procedure.
The sacroiliac joint connects the spine to the pelvis. It moves very little, probably only 3-5 degrees, and is slightly more mobile in females than males. It acts primarily as a shock absorber between the lower body and the trunk and in its construction is a synovial joint supported by the sacroiliac ligaments.
Pain from the sacroiliac joint is common, forms part of the differential of lower back pain and may be responsible for up to 30% of lower back pain. It is more common after trauma and also after pregnancy, here thought to be due to the changes in the pelvis around childbirth. Patients that have undergone lumbar spinal fusion, especially of the lumbo-sacral spine, seem to have a higher risk for sacroiliac joint dysfunction and pain. The same is thought to be true for patients that have had hip replacements. Inflammatory conditions around the sacroiliac joint, such as ankylosis spondylitis, can cause sacroiliac joint dysfunction but in this case is usually self-limiting and treated medically
The pain from sacro-iliac joint dysfunction can initially be managed with pain medication, physiotherapy and on occasion injections into or around the sacroiliac joint. Pain management may on occasion require denervation of the sacroiliac joint. The joint has both anterior and posterior innervation and where denervation should be focused depends upon exactly upon which nerves are being irritated. The lower back pain that comes from the sacroiliac joint is often unilateral and localised to the posterior pelvis rather than back and characteristically is worsened by transitioning from one position to another.
Fusion leads to improved pain relief, better quality of life, and less disability when compared to non-surgical treatment but carries of course the risks associated with surgery. Here in the UK Sacroiliac joint fusion is supported by NICE (National Institute for Clinical Excellence)guidelines which can be found at https://www.nice.org.uk/guidance/mtg39.
Sacroiliac joint fusion can be performed with a minimally invasive technique, and the most established of these is using the iFuse implant. The rationale behind minimally invasive surgery is reducing blood loss, reducing muscle damage, and allowing a shorter hospital length of stay.
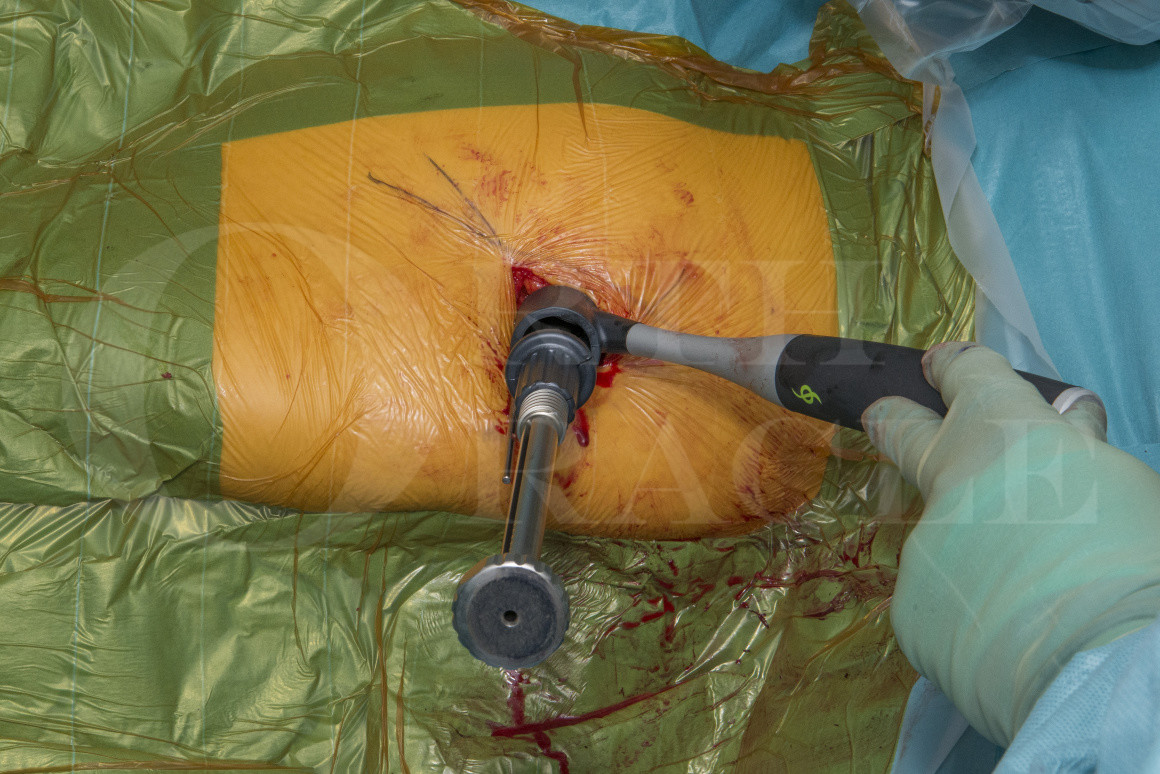
The iFuse is a triangular cross-section titanium implant and generally three titanium implants are required across the SI joint to fuse it. They are delivered using a cannulated delivery system with soft tissue protectors. This can be achieved using a navigation system or using a non-navigated technique as demonstrated in this OrthOracle technique.
The benefits of this system include bone on-growth and in-growth, for a robust fusion without need for joint preparation. The triangular shape does lend itself well to immediate stability of the fused joint when compared to round implants. The main other benefit for me is the wealth of data available for this particular implant including level 1 and 2 studies.
My sincere thanks to Mr Matthew Newton Ede, Consultant Spinal Surgeon, who collaborated with me both on the case and also production of the operative technique.
Author: Andrew Young FRCS (Tr & Orth)
Institution: The Royal Orthopaedic Hospital, Birmingham, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















