Subscribe to get full access to this operation and the extensive Spine Surgery Atlas.
FREE TRIAL
Learn the Scoliosis correction(neuromuscular): Anterior release and apical corpectomy surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Scoliosis correction(neuromuscular): Anterior release and apical corpectomy surgical procedure.
Neuromuscular scoliosis is the second most common type of spinal condition after Adolescent Idiopathic Scoliosis (AIS).
The term neuromuscular scoliosis describes a non-congenital spinal deformity that occurs in patients with any type of pre-existing neuromuscular diagnosis.
Patients with neuromuscular scoliosis remain a surgical challenge not only because of the spinal deformity but because these patients are of fragile overall health. It is for that reason such patients are best managed in centres with support from a multi-disciplinary team (MDT) since the spinal deformity is only one facet of their overall health needs.
It is important to appreciate that the term neuromuscular scoliosis includes a large number of underlying neurological diagnoses and pathologies and although the presentation of many of these patients with spinal deformity may be similar, subtle differences and complexities of the underlying medical condition limits complete generalisation when deciding on management.
That said, regardless of the underlying diagnosis, the later result of a progressive neuromuscular scoliosis deformity on a patient is similar. In many cases a large deformity will cause difficulties in daily care and positioning, ambulation (in ambulatory patients) and wheelchair positioning or sitting balance in those unable to walk or stand. Over time, the deformity may contribute to pain (costo-pelvic impingement), alterations in skin integrity (pressure sores) as well as pulmonary and cardiac compromise secondary to mechanical effects on thoracic volume and compliance.
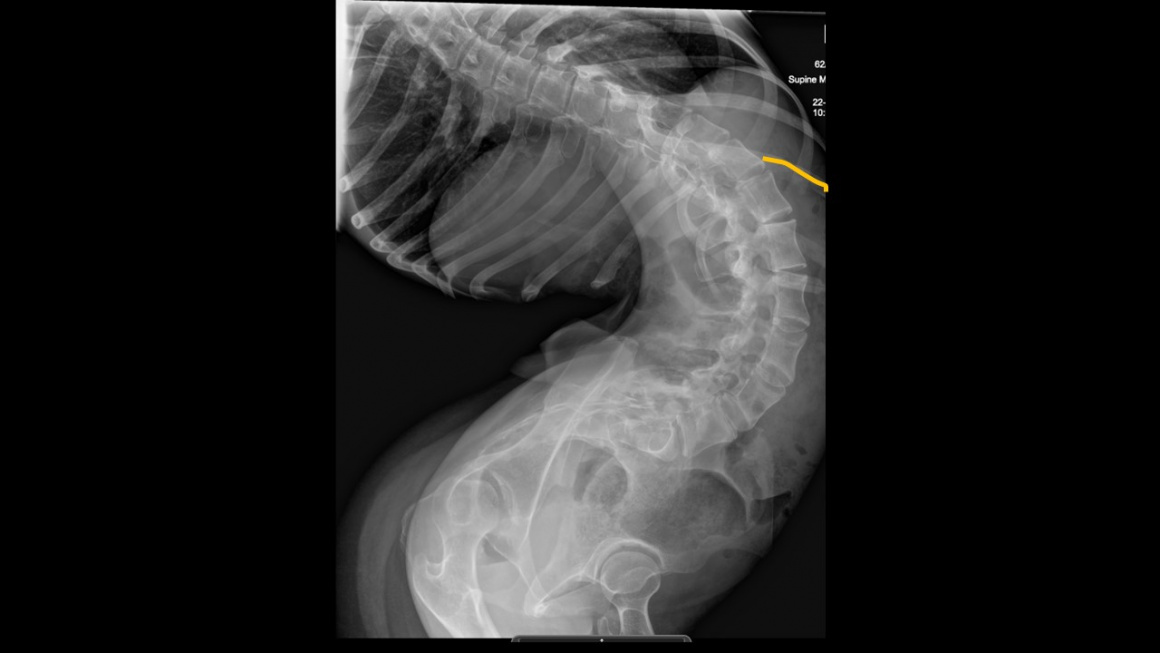
This case involves a patient with Cerebral Palsy who had a delayed referral to our institution and thus presented with a significant neuromuscular scoliosis.
Cerebral Palsy is the most common neuromuscular condition seen by orthopaedic surgeons. It results from a static upper motor neurone lesion that interferes with the developing motor system (before the age of 2 years). The lesion is usually caused by an anoxic injury in the perinatal period but child abuse (Non-accidental Injury) is another cause of a brain injury which can lead to cerebral palsy.
Cerebral Palsy subtypes include higher tone unilateral, higher tone bilateral, dyskinetic, ataxic or mixed types. The overall incidence of scoliosis in Cerebral palsy is 25% but the prevalence of scoliosis and the risk of being diagnosed with a moderate or severe scoliosis are related to the subtype and the Gross Motor Function Classification System (GMFCS). GMFCS is a classification 1-5 (1 -normal child, can walk, run, climb stairs etc; 2 – walk in most settings, struggles with balance on uneven ground/uses railings to climb stairs etc.; 3 – walks using hand-held mobility device and uses a wheel chair for longer distances; 4- require wheelchair predominantly but can stand and perhaps mobilise with help very short distances within the home; 5- wheelchair dependant and limited in their ability to maintain trunk and head postures).
Spasticity, muscle weakness, and incomplete muscle control contribute to impaired trunk control and the development of spinal deformity. As children grow their body increases in size and weight. Usually these additional forces acting on the growing spine are balanced by symmetrical muscle activity however, this does not occur in children with cerebral palsy. A vicious cycle of pathological muscle tone, increasing curvature and subsequent secondary inhibitory vertebral growth disturbances in the concavity of the curve fuels curve rigidity, as well as progressive vertebral and spinal deformity.
The risk of developing a scoliosis, and the risk of a more severe scoliosis, is related to age of first presentation and GMFCS level.
The majority of scoliosis progression is seen to occur during child and adolescents growth, in-particular during the adolescent pubertal growth spurt. Further progression of scoliosis has been reported in adults with cerebral palsy with a range between 1.4 degrees and 4.4 degrees per year.
The more severely a child is affected, the higher the risk for developing a scoliosis, and, progression of that scoliosis. At the most severe end of the spectrum, a child with cerebral palsy who cannot sit independently (GMFCS 5) may have a risk as high as 90% for developing a scoliosis, compared to a child with cerebral palsy who walks where the risk of developing a scoliosis is very much less. The scoliosis often develops between 6 and 10 years of age. It is flexible initially but tends to become stiffer with time.
A major complication rate of 36% has been reported following spinal deformity surgery in patients with cerebral palsy, with a spine-related re-operation rate of 14.0%. In a published series of 257 patients with cerebral palsy, 24.9% of complications occurred in the peri-operative period and 7% of patients had more than one complication. The most common complications were wound (6.2%) and pulmonary issues (10.9%), deep wound infections (3.1%) and instrumented related complications (2.3%). 4.3% of patients died between 3 months and 5.6 years post-operatively (36% of those deaths were within a year of surgery and 18% directly related to the spinal deformity surgery).
Case:
For the most part, correction of a neuromuscular scoliosis involves a long posterior fixation, possibly into the pelvis, having preformed a posterior column release and osteotomies before instrumentation. Occasionally an anterior release is needed prior to posterior surgery. If an anterior release is required, it is best done on the same day as the posterior surgery. I don’t believe a curve of the magnitude this patient presented with can be reliably, and safely, corrected in a single staged operation. Patients with neuromuscular scoliosis will often be osteopenic or osteoporotic and applying a large force when attempting an instrumented correction can result in failure at the metal/bone interface. In this patient, even if one was confident they could correct the spinal deformity in a single operation, the skin and underlying soft tissues may be too contracted to reliably close following correction. For those reasons, I opted for a staged correction.
The surgical strategy, having liaised with the wider MDT team and my plastic surgical colleagues, was to apply longitudinal traction to the patient for a period of several weeks to initially determine curve stiffness and begin stretching out contracted soft tissues at the concavity side of the curve; assuming the curve was stiff and soft tissue contracted [most likely scenario] this would be followed by an anterior release and apical corpectomy (removal of anterior vertebral body and pedicles to the level of transverse processes) with the possibility of a apical posterior release and completion of apical vertebrectomy (removal of remaining osseous components of apical vertebra) if curve remained stiff; we would subsequently apply further traction for a 2-4 week period (HALO – Gravity, so as to allow patient to sit up and sit out of bed) before performing the final definitive posterior instrumented correction and fusion.
We applied a HALO ring to the patient’s head and inserted a distal femoral pin into both distal femur’s two weeks prior to the anterior release and apical corpectomy. This allowed application of longitudinal traction in bed before the anterior release and apical corpectomy. I will present that operation in this module. The anterior thoraco-lumbar approach to the spine was sub-diaphragm since I only needed to expose the discs of T11/12 to L4/5. To see a thoraco-lumbar approach in-which the diaphragm is taken down to aid spine exposure read the OrthOracle technique:
OrthOracle readers will also find the following related instructional techniques of interest:
Author: Neil Upadhyay FRCS(Tr & Orth)
Institution: The Avon Orthopaedic centre, Southmead Hospital, Bristol, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu