Hallux Rigidus: Youngswick osteotomy
Overview
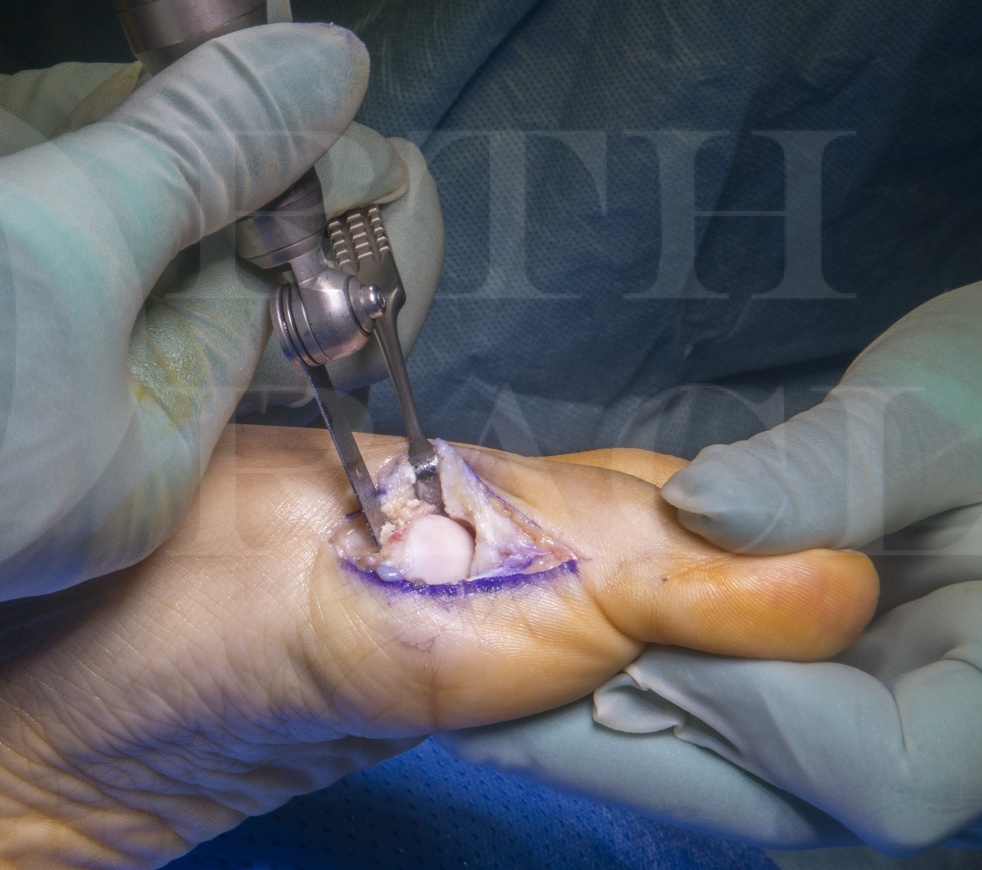
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Hallux Rigidus: Youngswick osteotomy surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Hallux Rigidus: Youngswick osteotomy surgical procedure.
The aetiology of hallux rigidus is multi-factorial. Causes include trauma, osteochondritis dissecans, inflammatory arthropathy and iatrogenic injury. A proportion of cases are thought to be related to metatarsus primus elevatus. This was first noted by Lambrinudi In 1938 who described impingement pain and progressive degenerative change result from a mechanical malalignment of the 1st metatarso-phalangeal joint, with an eccentrically located centre of rotation of the 1st metatarsal head. Patients will frequently present with a reasonable range of movement in the non-loaded foot at the 1st MTP joint but a notable restriction in movement in the loaded foot, sometimes called a “functional hallux limitus”. Radiographic findings in metatarsus elevatus, are of a variable degree of degenerative change within the joint, and on the lateral weight bearing view, the proximal phalanx lies in a flexed position relative to the metatarsal head, and the 1st metatarsal is elevated relative to the lesser metatarsals. Patients may present with a dorsal prominent at the 1st metatarsal head which is out of proportion to the small or absent dorsal osteophyte.
Austin first described a distal shortening planterising osteotomy for the treatment of metatarsus primus elevatus in 1962. Youngswick modified the Austin technique to allow a plantarisation and proximalisation of the 1st metatarsal head, which he described in 1982. A number of other distal metatarsal osteotomies including the Watermann-Green osteotomy, the V-osteotomy and Weil’s osteotomies have been described to address the problem.
Bryant in 2004 treated 23 feet with mild to moderate hallux limitus with 2 years of follow-up and found that the Youngswick osteotomy produced a significant increase in the range of movement and dorsiflexion in the 1st MTP joint in patients with mild to moderate hallux limitus. They found that pressure measurement showed peak pressure beneath the hallux of the 1st metatarsal remained unchanged. However, peak pressure was significantly increased through the 2nd metatarsal and reduced in the 5th metatarsal, the concluded that post-operatively the foot functioned in a less inverted and more physiological pattern, and that the procedure was associated with a high patient satisfaction.
Lemar in 2006 provided a mechanical comparison of the Youngswick versus the modified Weil’s osteotomy and sagittal V osteotomy and noted that the Weil’s and Youngswick osteotomies were mechanically more stable than the sagittal V osteotomy when loaded to failure.
In a journal of foot and ankle surgery 2016, Slullitel looked at 78 patients who had undergone a Youngswick osteotomy for stage 2/3 hallux rigidus and assessed the 1st metatarsal length as being longer, equal or shorter than the 2nd metatarsal pre-operatively. They recorded high patient satisfaction. 97% of patients would recommend the procedure to family members. There was no difference between the groups in relation to transfer metatarsalgia or complication rates. They concluded that the procedure had high satisfaction rates, independent of 1st metatarsal length.
Villadot In ‘the foot’ 2017, reported the study involving 50 patients, 25 who underwent a Youngswick Austin osteotomy versus distal oblique osteotomy, they found that both the Youngswick osteotomy and distal oblique osteotomy are both safe, stable with good to excellent clinical results and low complication rate. Slightly higher patient satisfaction not statistically significant in the oblique osteotomy group.
The Youngswick plantarising shortening 1st metatarsal osteotomy is a useful surgical adjunct for management of hallux rigidus in mild to moderate hallux rigidus, especially useful in those patients with a metatarsus elevatus and a well preserved range of movement in the unloaded foot compared to the loaded foot.
References:
Modifications of the Austin Bunionectomy for treatment of metatarsus primus elevatus associated with hallux limitus. J Foot Surg. 1982 Summer;21(2):114-6. Youngswick FD.
J Am Podiatr Assoc. 2004 Jan-Feb;94(1):22-30. Plantar pressure and joint motion after Youngswick procedure for hallux limitus.
Bryant AR, Tinley P, Cole JH.
J Foot Ankle Surg. 2016 Nov-Dec;55(6):1143-1147. Joint Preserving Procedure for Modrate Hallux Rigidus: Does the Metatarsal Index Really Matter?
Slullitel G, Lopez V, Seletti M, Calvi JP, Bartolucci C, Pinton G.
Youngswick-Austin versus distal oblique osteotomy for the treatment of Hallux Rigidus. Foot(Edinburgh). 2107 Aug;32:53-58.
Viladot A, Sodano L, Marcellini L, Zamperetti M, Hernandez ES, Perice RV.
Author: Nick Cullen FRCS (Tr & Orth)
Institution: The Royal National Orthopaedic Hospital, Stanmore, London,UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















