Posterior Ankle decompression-Arthroscopic technique
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Posterior Ankle decompression-Arthroscopic technique surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Posterior Ankle decompression-Arthroscopic technique surgical procedure.
Posterior ankle impingement may occur as a result of an acute injury such as an ankle sprain, or as a result of repetitive trauma. The anatomy of the posterior ankle plays an important role in the syndrome. The most common predispositions tend to be osseous, such as an Os Trigonum, a Steida process, a prominent posterior tibial plafond or a posterior tibial osteophyte, or. Less frequently the impingement is soft tissue, related to a thickened posterior capsule, scar tissue or calcific bodies. The common feature of all these pathologies is that they predispose to compression during plantar flexion.
The most common cause of posterior impingement is the Os Trigonum, The ossific Os appears between 7 and 13 yrs of age and fuses to the body of the talus within 1-2 years, forming a trigonal (steida) process of varying size. In 10% of patients, it remains a distinct ossicle. The Os Trigonum can become symptomatic due to abutment between calcaneum and tibia, or due to disruption of the fibro-cartilagenous synchondrosis.
Repetitive impingement can lead to thickening of the posterior capsule, the intermalleolar ligament or the posterior talo-fibular ligament.
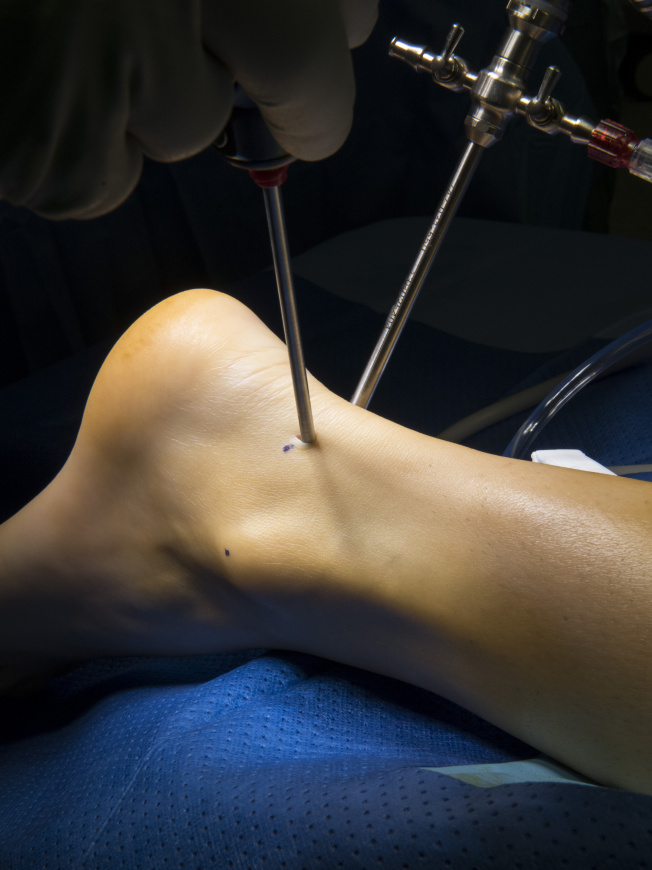
Various pathologies are related to the posterior ankle and subtalar joint. Arthroscopic access to the anatomical region is a useful tool in the surgeons armoury. The arthroscopic approach to the posterior ankle is advantageous, as it provides excellent visualisation to all of the posterior ankle and subtalar joint and FHL tendon, whilst the smaller surgical insult, when compared to open surgery, leans itself towards accelerated rehabilitation.
the structures at risk during the surgery, include the achilles tendon, the flexor hallucis longus tendon, the sural nerve and the tibial nerve, and a comprehensive understanding of the anatomy of the posterior ankle is important when plotting ones approach.
The posterior portals provide good access to the posterior ankle and subtalar joint. The posterior facet of the subtalar joint is not traversed by ligamentous structures, and normally can be clearly identified, however when there is a large steida process or Os Trigonum, the view will be obscured. Access to the posterior ankle joint however is obscured by the posterior Talofibular, tibiofibular ligament and the posterior inter malleolar ligaments, and access must be gained between these ligaments.
Parisien first described the technique to assess the posterior subtalar joint in 1985, this was popularised by Van Dijk in 2000 when he reported successful posterior arthroscopic treatment of a Ballerina presenting with an Os Trigonum and FHL tendinosis.
Author : Mr Nick Cullen FRCS (Tr & Orth)
Institution :The Royal National Orthopaedic Hospital ,Stanmore ,UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















