Hallux valgus: Technical tips for closure
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Hallux valgus: Technical tips for closure surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Hallux valgus: Technical tips for closure surgical procedure.
Patients with symptomatic Hallux Valgus will have pain predominantly from the medial eminence, though of course not all patients are symptomatic. Pain can also occur from the relative overload of the second and third MTP joints, occurring secondary to the de-functioned first ray that happens with a bunion. Pain is classically only when in shoe-wear (or more specifically tighter fitting shoe-wear), so if pain occurs when weight-bearing out of shoes exists one should consider an intercurrent diagnosis such as Hallux Rigidus. Surgery is mainly indicated for pain, though on occasion cosmetic correction may be appropriate, dependent upon the extent of the patients limitations due to appearance of the foot and a thorough appreciation of the pros and cons of surgery and recovery.
With regards to radiographic criteria a mild Hallux Valgus could be said to be a Hallux Valgus angle (the degree of lateral angulation of the hallux relative to the first ray ) of less than 2o degrees and an inter-metatarsal (IM) angle of less than 11 degrees. A moderate deformity displays a Hallux Valgus angle of 20 to 40 degrees and an Inter-metatarsal angle of 11-18 degrees. A severe deformity a Hallux Valgus angle in excess of 4o degrees and inter-metatarsal angle over 18 degrees.
The principle steps of all surgical correction require both lateralising the medially displaced first metatarsal and rebalancing the MTP joint capsule, which is stretched medially and contracted laterally. Both these steps inevitably leave excess medial soft tissue, the greater the deformity corrected then the more soft tissue resulting. Often this is simply left and included in the closure.
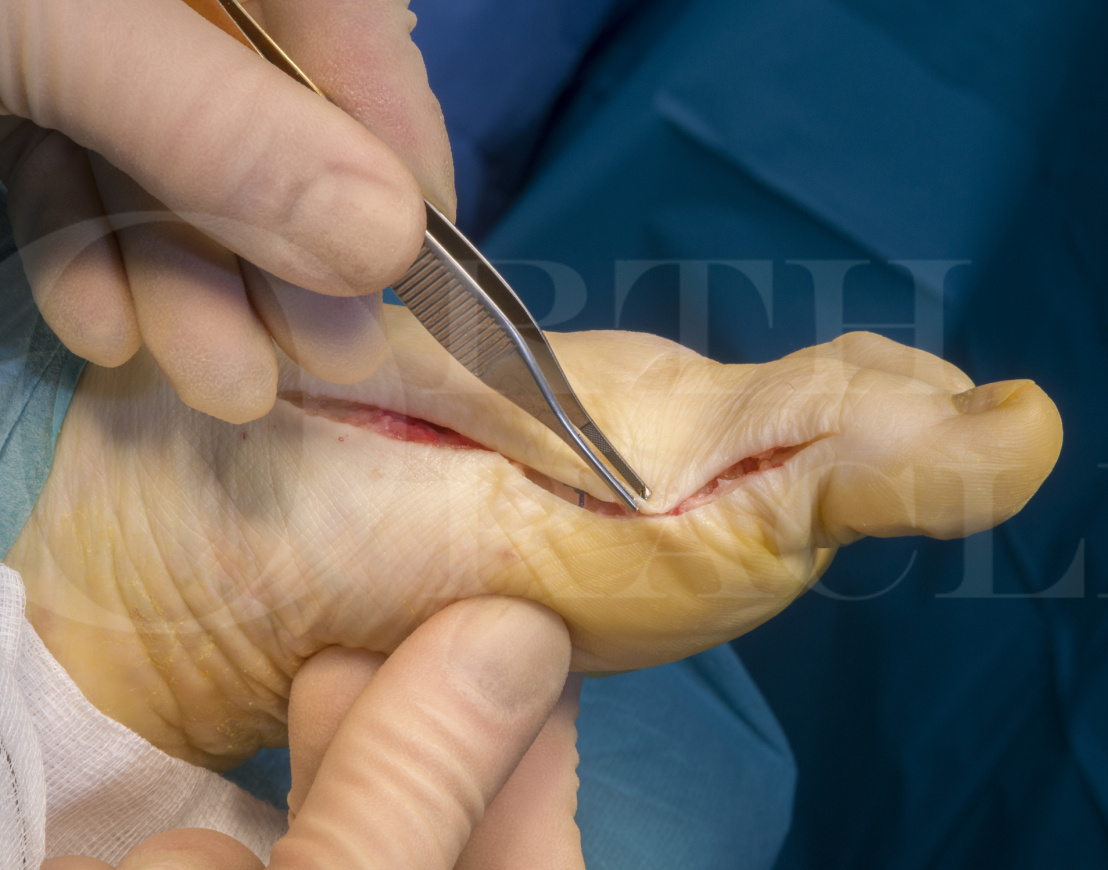
My own practice has been to aggressively excise both capsule and skin, whilst paying attention to the cutaneous nerves that sit in close proximity. This assists the corrective closure, reduces the inevitable sloughing of excess soft tissue if left and also gives a much better immediate post-operative appearance. It’s also a small thing to do.
The capsular closure suture technique that I also detail here I don’t think can be bettered, and was taught to me by one of my mentors, Professor Michael M Stephens from Dublin. The capsular excision and skin advancement aspects are my own contributions.
OrthOracle readers will also find the following instructional techniques of interest:
Hallux valgus: Lateral MTP joint release ( modified McBrides procedure
Hallux valgus: Chevron Osteotomy
Hallux valgus: Scarf osteotomy
Author: Mark Herron FRCS
Institution: OrthOracle, London, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















