Revision total hip replacement: MUTARS proximal femoral endoprosthesis (Implantcast)
Overview
Subscribe to get full access to this operation and the extensive Hip Surgery Atlas.
Learn the Revision total hip replacement: MUTARS proximal femoral endoprosthesis (Implantcast) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Revision total hip replacement: MUTARS proximal femoral endoprosthesis (Implantcast) surgical procedure.
Periprosthetic joint infection (PJI) is a devastating complication of prosthetic joint replacement, accounting for 13.8% of 15,923 of re-revision total hip arthroplasties performed in the UK in 2018, as detailed in the 16th annual National Joint registry report. More common indications for revision surgery include aseptic loosening (43.5%), pain (16.9%), instability (14.4%), osteolysis (14%), and other important but less common indications for re-revision include implant wear (12.6%) and periprosthetic fracture (10.1%). Both instability and infection are much more common indications for a second revision than first revision hip replacement, highlighting the increased risk of instability and infection following the first revision of a hip replacement compared to that of primary hip replacement
(https://reports.njrcentre.org.uk/Portals/0/PDFdownloads/NJR%2016th%20Annual%20Report%202019.pdf).
Surgical management involves identification of the infecting pathogens and optimisation of the host prior to major surgery, which may involve debridement and implant retention, or a single or two-staged revision procedure. Staged revision surgery remains the gold standard of care for multiply revised infected hip replacements. At the first stage the prosthetic components are explanted and the involved soft-tissues are radically debrided. The joint is temporarily stabilised with either an articulating cement spacer, as in this case, or non-articulating spacer for approximately three months. At the second stage, following repeat debridement, the joint is reconstructed.
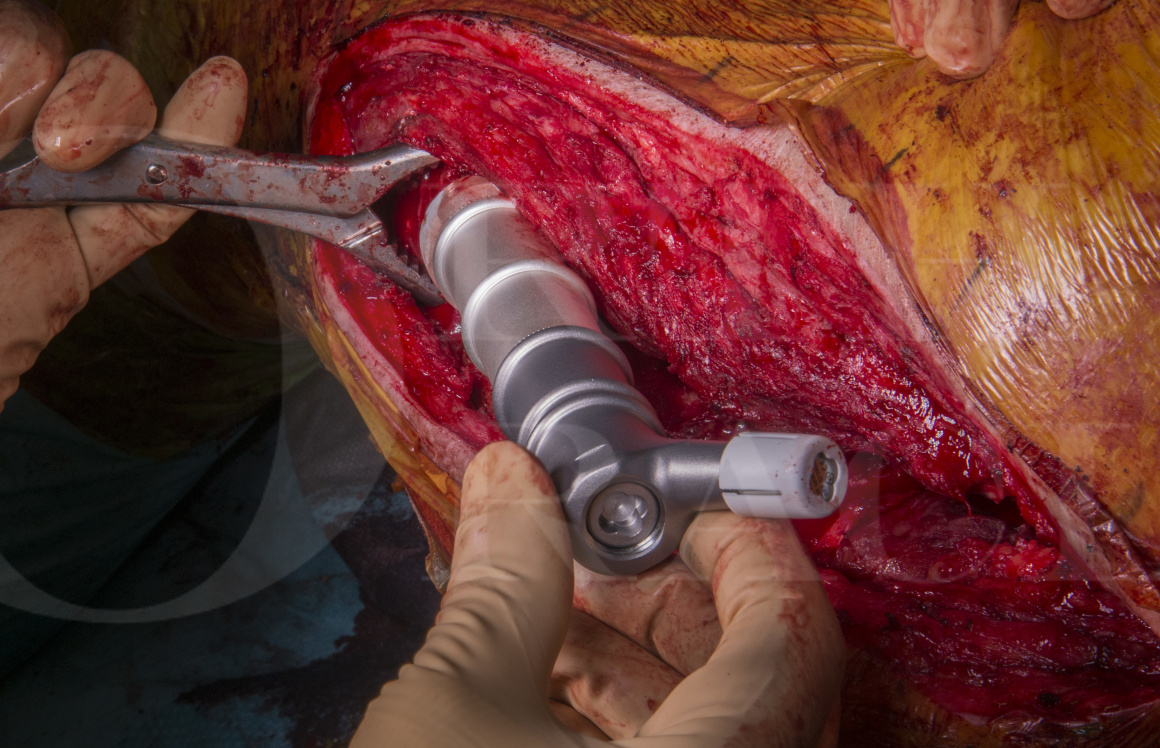
To minimise the risk of PJI relapse I prefer a silver coated modular proximal femoral endoprosthesis with cemented medullary stems (MUTARS, Implantcast, Buxtehude, Germany). To minimise the risk of acetabular failure due to aseptic loosening I use a trabecular metal revision system (Trabecular Metal Acetabular Revision System, TMARS, Zimmer Biomet, Warsaw, Indiana, US) which allows the use of a full range of liners, augments, cages to address almost all acetabular defects. To minimise the risk of dislocation I have chosen a dual-mobility articulation in this case.
Readers will also find the following techniques of interest:
Revision Total Hip replacement: Stryker custom acetabulum and SERF Dual mobility Hip (De Puy)
Revision Total Hip replacement: Direct exchange Link MP revision stem for periprosthetic fracture
I am grateful to Mr Mike Parry FRCS (Tr & Orth) for the images used in this technique.
Author: Jonathan Stevenson FRCS (TR & Orth)
Institution: Royal Orthopaedic Hospital, Birmingham, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















