Suprascapular nerve decompression and reconstruction
Overview
Subscribe to get full access to this operation and the extensive Upper Limb & Hand Surgery Atlas.
Learn the Suprascapular nerve decompression and reconstruction surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Suprascapular nerve decompression and reconstruction surgical procedure.
A 35 year old man was referred to the regional peripheral nerve injury service 10 months after a heavy blow to the front of the left shoulder during a fall from a mountain bike during an off road descent. Plain radiographs of the clavicle and shoulder were reported as normal. He was rehabilitated with physiotherapy. After 3 months there was useful abduction using deltoid but no evidence of supraspinatus function and he was referred for an ultrasound of the rotator cuff to exclude a tear. The ultrasound was normal showing mechanical integrity of the muscle-tendon unit. Further rehabilitation was advised. The treating physiotherapist highlighted weak abduction and external rotation and a diagnosis of suprascapular nerve neurapraxia was made. No neurophysiology was requested to confirm this diagnosis. He was not improving by 9 months with weak overhead activity and poor external rotation and he was referred to the nerve unit for assessment.
He was assessed 10 months after the injury and there was no function in the supraspinatus or infraspinatus with wasting of both muscles. There was deep seated pain over the suprascapular nerve on palpation. The remainder of the brachial plexus examination was normal. There was no Tinel’s sign at the upper trunk which would have been suggestive of an avulsion of the suprascapular nerve take-off at this level. However the suprascapular nerve is has no cutaneous sensory territory and Tinel’s sign for a rupture is therefore unreliable. A diagnosis of traction injury or distal rupture of the suprascapular nerve was made and he was listed for urgent exploration the next day. Intra-operative neurophysiology was planned to avoid further delay. Effective reinnervation in a proximal rupture will only be achieved with a nerve transfer at this stage. The time of presentation is too late for a proximal graft reconstruction to provide useful reinnervation by 12 months. The best option for the patient would be to identify evidence of traction injury with axonopathy and regeneration complete but non-functioning due to persisted segmental conduction block at a tight suprascapular ligament. In such cases stimulation improves after decompression of the ligament and further expectation of recovery and strengthening for 6-12 months would be anticipated. If a short segment rupture is identified at the suprascapular notch this would be amenable to a graft. Otherwise the recommended treatment would be a decompression, stimulation assessment and consideration given to a nerve transfer.
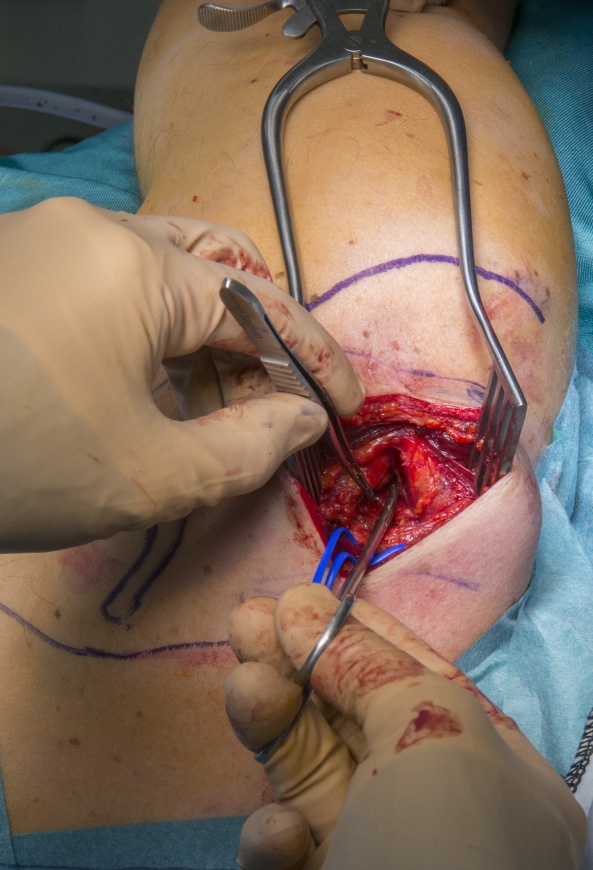
At surgery there was a tight ligament but no stimulation and no neuroma at the area exposed. A working diagnosis of a more proximal rupture was made and a distal nerve transfer from the medial branch of the XIth cranial nerve was performed just proximal to the suprascapular notch.
Author: Dominic Power FRCS Orth, Consultant Hand and Peripheral Nerve Surgeon
Institution: Peripheral Nerve Injury Service, Queen Elizabeth Hospital, Birmingham, UK
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















