Ankle fracture: Arthrex tightrope for acute syndesmotic injury and Stryker Variax plate for fibula fracture
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Ankle fracture: Arthrex tightrope for acute syndesmotic injury and Stryker Variax plate for fibula fracture surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle fracture: Arthrex tightrope for acute syndesmotic injury and Stryker Variax plate for fibula fracture surgical procedure.
The distal tibiofibular syndesmosis is a unique syndesmotic joint, powerfully bound by a variety of ligaments to maintain the integrity of the ankle mortise. The distal anatomy of the two bones are created in such a way that the medial surface of the distal fibula fits into a groove on the lateral surface of the distal tibia called the incisura fibularis which offers the bony stability to this joint. The anterior part of this joint is stabilised by the Anterior Inferior Distal Tibio-Fibular ligament (AITFL), the posterior aspect by the Posterior Inferior Distal Tibio-Fibular ligament (PITFL) and the transverse Tibio-Fibular ligament. Directly between the contiguous surfaces of the tibia and fibula is the interosseous ligament which extends throughout the length of the fibula.
The PITFL is by far the strongest ligament in this complex and is the least likely to be ruptured. Once ruptured however it is most likely to be associated with severe rotational or dislocating injuries of the ankle and associated ankle instability.
The syndesmotic ligaments stabilise the fibula with respect to both talus and tibia, whilst allowing a degree of rotation of the fibula, required in particular during full ankle dorsiflexion when the widest portion of the talus comes into the mortise. As with any ligament injury the key point is not solely whether these ligaments have been injured, but rather their stability in determining the need for treatment. If instability is not addressed, high contact pressures at the joints surface ensue and early degenerative change occurs in most patients.
Traditional fixation of unstable syndesmotic injuries has been with two parallel, non-compressive, small fragment screws placed across the ankle at the level of the tibial incisura. Such fixation also requires a decision as to whether the screws need to be removed and furthermore, the optimal timing for such removal.
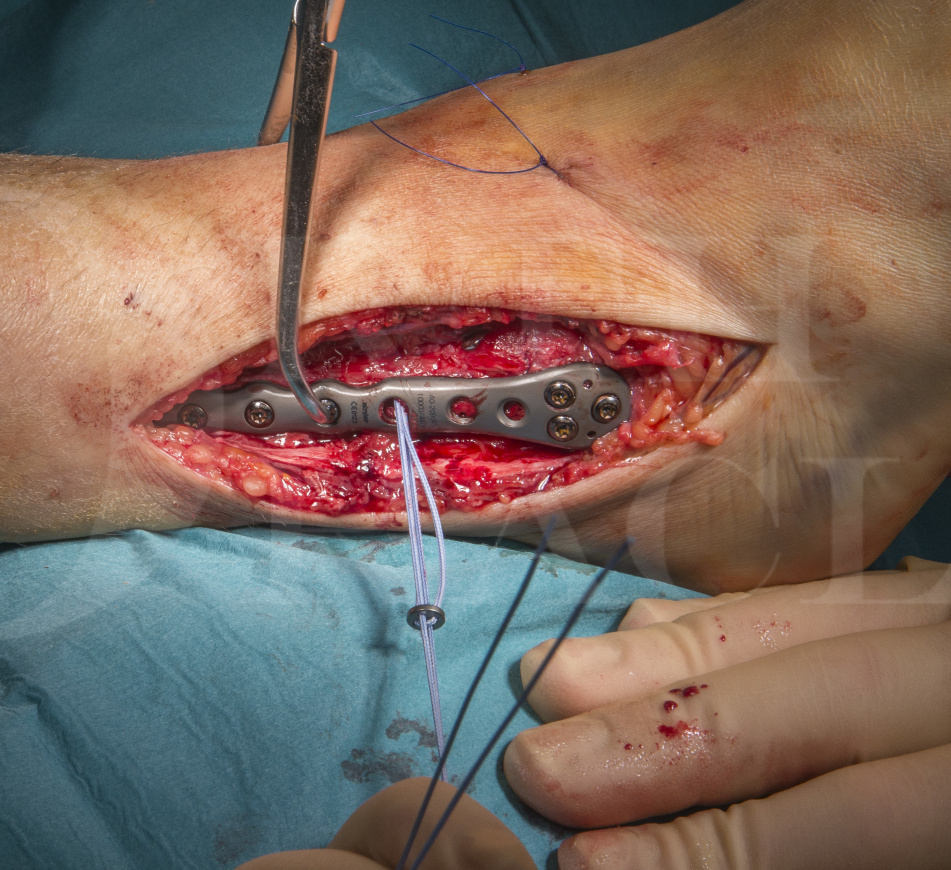
The use of a Arthrex tightrope implant, is far more physiological in terms of the way the syndesmosis is held, allowing more normal movement at the ankle mortise. It is a simple and ingenious implant that has proved its worth not only in syndesmotic ankle reconstruction but also in the shoulder and forefoot. It consists of two metal buttons that rest on the respective bony surfaces to be approximated, and a robust four stranded Fibrewire suture construct which links these buttons. The design allows easy apposition of the buttons towards each other by the effective “slip-knot” set up of the suture strands.
Readers will also find of use the following OrthOracle techniques:
Internal fixation of ankle fracture : Fibula pro-tibia fixation technique with Stryker Variax plate.
Internal fixation of medial malleolar ankle fracture with ASNIS screws
Lateral malleolar fixation using Acumed Fibula Rod System
Postero-lateral plating of pronation-external rotation ankle fracture (posterior malleolar fixation)
Fusion of the syndesmosis for isolated distal tibio-fibular arthritis
Author: Mark Herron FRCS
Institution: The Wellington Hospital, London, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu
Online learning is only available to subscribers.



















