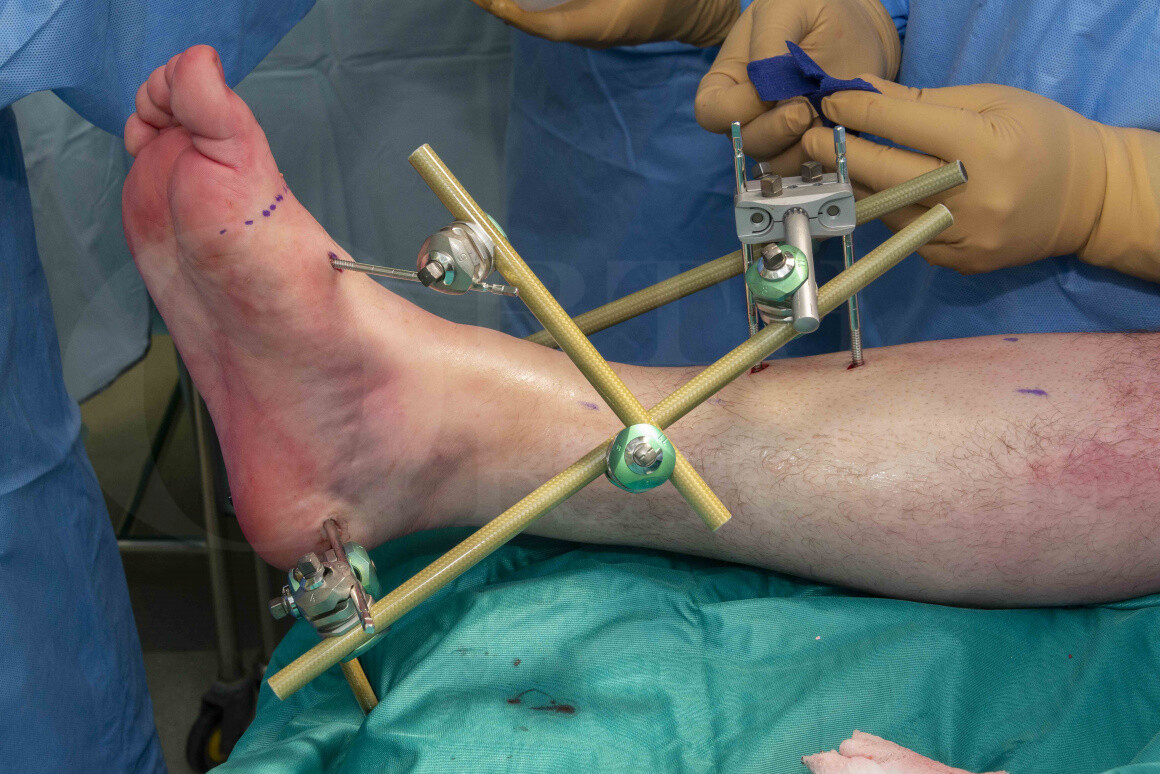
Ankle fracture: Stabilisation with Hoffmann 3 Ankle-spanning External Fixator (Delta frame)
Overview
Subscribe to get full access to this operation and the extensive Foot Surgery Atlas.
Learn the Ankle fracture: Stabilisation with Hoffmann 3 Ankle-spanning External Fixator (Delta frame) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle fracture: Stabilisation with Hoffmann 3 Ankle-spanning External Fixator (Delta frame) surgical procedure.
Ankle external fixation is an essential procedure that needs to be second nature for any surgeon undertaking acute trauma cases. Although ankle fractures are common, the vast majority do not need to be treated with a temporary spanning external fixator because they are usually low energy, closed injuries. Ankle spanning external fixators are indicated for higher energy injuries where there is a need to “span, scan and plan” i.e. a pilon fracture; an open ankle fracture; a talar body dislocation, or those where there are significantly traumatised soft tissues. Having said that, the first step in your treatment algorithm should be immediate joint / fracture reduction and application of a plaster of Paris backslab. In grossly unstable injuries, those that cannot be reduced, those where fracture length cannot be maintained or those that require soft tissue monitoring, then a spanning external fixator is a better option.
The British Orthopaedic Association Standard for Trauma (BOAST) recommends for unstable ankle fractures in the under 60 age group early operative fixation (i.e. < 24 hours). In the over 60 age group, providing a satisfactory reduction can be achieved and maintained, then a close contact cast is an option. The guidelines state that the use of external fixation may be rarely indicated in the presence of gross instability associated with soft tissue compromise. This therefore implies that patient’s with a fracture dislocation, older than 24 hours that cannot be reduced and maintained in a plaster of Paris, should be considered for a spanning ankle external fixator. It is my experience, that patients between 24-48 hours can have an evolving injury and the swelling may still be on the way up. This means that if a plaster backslab is applied, it may need to be released due to ongoing swelling and the fracture reduction is lost.
There are also a cohort of patients that as the swelling decreases, the plaster backslab becomes loose and the fracture re-displaces and thus the swelling persists. There’s a final group that due to repeated soft tissue inspection, the plaster backslab becomes weaker / looser and again the fracture re-displaces and the swelling persists. In general, if a patient still has significant swelling at day 5 post reduction, then I’d recommend checking with an x-ray, as occasionally the fracture has subluxed and this can also happen while in an external fixator depending on the stability of the construct.
The Hoffmann 3 external fixation system was developed for use in acute trauma, “damage control” orthopaedics and also for definitive fixation. It has a variety of features that make it simple, fast to apply and adaptable for many types of patients and injury patterns. It is indicated for stabilisation of open and/or unstable fractures and where soft tissue injury may preclude the use of other fracture treatments e.g. casts, intramedullary devices or internal fixation. Additional indications include:
- Bone fracture fixation
- Osteotomy
- Arthrodesis
- Correction of deformity
- Revision procedure e.g. infection
- Bone reconstruction procedures
The Hoffmann 3 system is MRI Conditional up to 3.0 Tesla. This means that patient’s with this type of fixator can go into an MRI scanner providing certain conditions are met e.g. the field strength does not exceed 3.0 Tesla, and the MRI scan is performed in accordance with the testing schedule as specified by the manufacturer. The Delta couplings are fully compatible with the Hoffmann II MRI and the Hoffmann II Compact MRI. This means that you can use any combination of 5mm, 8mm and 11mm connecting rods.
OrthOracle readers will also find the following associated operative techniques of interest:
Minimally invasive distal tibial osteotomy and correction of deformity with the Taylor Spatial Frame
Compartment fasciotomy and Hoffmann 3 spanning external fixator for open tibial fracture
Tibial fracture non-union correction using Taylor Spatial Frame (Smith and Nephew)
Distal radius fracture: Compound injury stabilised with Hoffman II External Fixator
Author: Ross Fawdington FRCS (Tr & Orth)
Institution: The Queen Elisabeth Hospital, Birmingham, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















