Pelvic fracture fixation: Fixation of Sacroiliac joint diastasis using Brainlab navigation system
Overview
Subscribe to get full access to this operation and the extensive Hip Surgery Atlas.
Learn the Pelvic fracture fixation: Fixation of Sacroiliac joint diastasis using Brainlab navigation system surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Pelvic fracture fixation: Fixation of Sacroiliac joint diastasis using Brainlab navigation system surgical procedure.
Pelvic fractures occur in two major cohorts, the young and the old. The younger subgroup are in the main male patients who have suffered high energy accidents and who have good bone quality. These fractures are accurately described by the AO classification system. The second subgroup comprises older patients suffering from low energy trauma and who have poor bone quality. These osteoporotic fractures of the pelvis are increasing in frequency with ageing populations, and despite shared fracture patterns with the high energy group are usefully thought of distinctly as Fragility Fractures of the Pelvis (FFP), in terms of their management.
In young male polytrauma patients a sacroiliac diastasis indicates a more complex and less stable fracture pattern, whereas its presence in an FFP injury does imply major soft tissue disruption and the fracture displacement in these patients is minimal. Moreover, hemodynamic instability is unlikely in FFP fractures so the primary therapeutic target for these type of fractures are pain management and early mobilisation.
This OrthOracle surgical technique describes in detail fixation of a classic Fragility Fractures of the Pelvis (FFP) using the Brainlab 3D navigation system.
Conservative therapy may be an option for patients with FFPs who do not suffer from significant pain during early mobilisation. Hence, an attempt at pain medication and assisted mobilisation is a reasonable initial option in many Fragility Fracture of the Pelvis (FFP). However if this does not allow safe and effective mobilisation, early surgical fixation is indicated. My own preference is to use a minimally invasive approach, which reduces blood loss and soft tissue complications especially in situations which do not require extensive reduction manoeuvres.
The classical surgical therapy for undisplaced fractures is sacroiliac screw insertion which is guided by inlet, outlet and true lateral fluoroscopic imaging projections of the pelvis, and the exact placement of these screws depends on the anatomic position of the injury. In the case of a sacroiliac joint disruption, a partially threaded compression screw is used perpendicular to the joint line whereas trans-foraminal fractures are stabilised using fully threaded screws. Not all fracture patterns can be managed with minimally invasive techniques though. High energy fractures may also require posterior plates and a sacroiliac dislocation usually requires open reduction from an anterior approach but has a high risk of neurovascular complications including presacral plexus injuries.
This classical minimally invasive technique uses conventional fluorscopic imaging, where it is clear that the success of fixation and frequency of major complications is largely determined by the quality of visualisation. In many patients fluroscopy works well, but there are real technical challenges for visualisation imposed by very obese patients as well as the elderly with osteoporotic bone, both of which make identification of key bony landmarks very challenging (if not impossible). In these cases especially a navigated technique using 3D guided instruments overcomes the limitations of traditional image intensification, though of course navigation can be used for all cases if preferred.
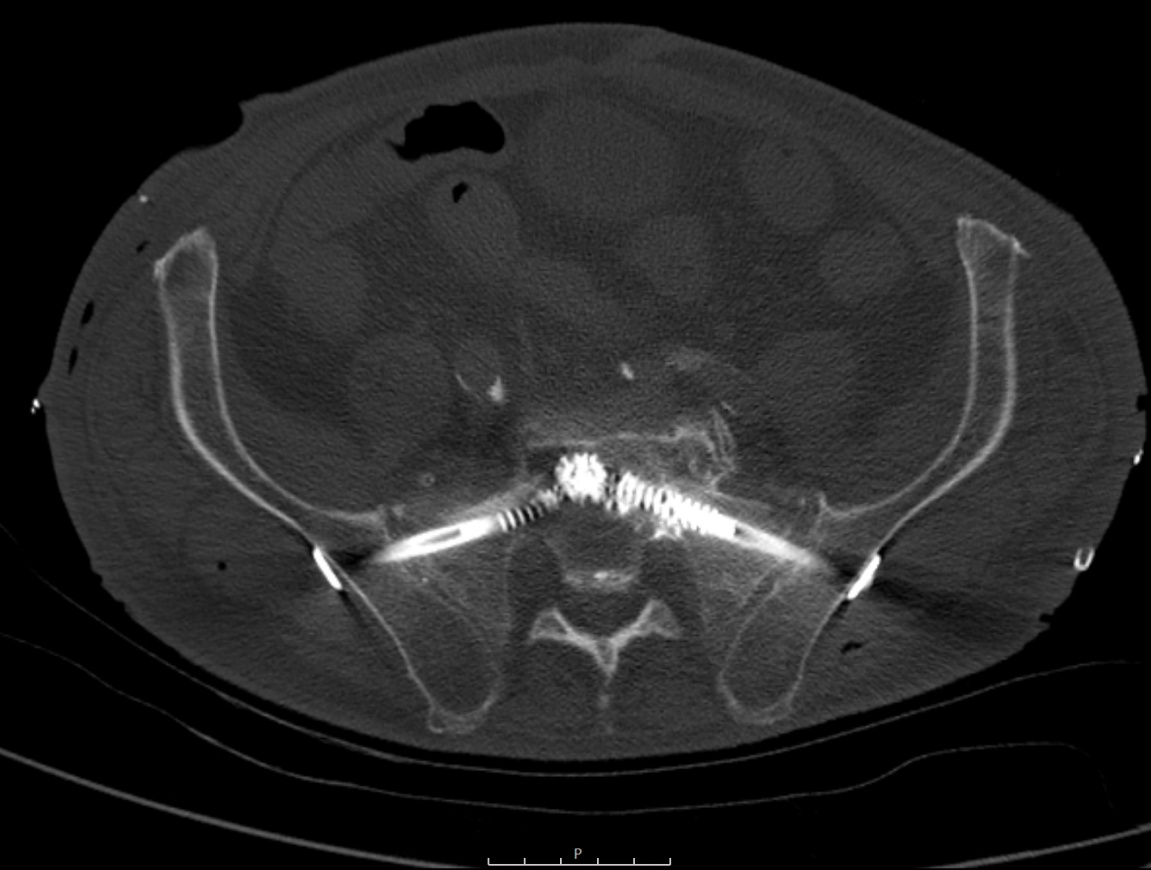
My preference is to use the navigation system from Brainlab, in combination with an on-table Siemens Cios 3D scanner. The workflow is pretty straight forward: first, we insert a reference tool on the contralateral anterior iliac spine, then we reference all instruments, then we drive a 3D scan of the region of interest, in this case the sacroiliac joint. Then, if necessary, we perform reduction and transient fixation using a 2.5mm K-wire, then we scan again. If everything looks well reduced, we then drill the screw using the navigation drill guide tool which shows the calculated trajectory inside the S1 body. The drill is left in place to perform conventional inlet/outlet views that verify its position, followed by a cannulated screw insertion, controlled again using inlet/outlet views and augmented with PMMA cement. Suero et al published a cadaveric study in Injury in 2021 which they demonstrated that one single PMMA augmented SI screw has similar biomechnical stability to 2 non augmented S1/2 screws. Bearing the risk of neuro-foraminal injury with each sacral screw used in mind, this demonstrates the value of being able to achieve appropriate surgical fixation with a single cement-augmented screw on each side, rather than two.
OrthOracle readers will also find the following associated pelvic and navigated surgical techniques of interest:
Sacro-iliac joint fusion, minimally invasive technique with iFuse implant.
Total Knee replacement: Mako Triathlon robotic assisted cruciate retaining TKR (STRYKER)
Total Knee replacement: MAKO robotic triathlon cruciate substituting knee replacement
Total Hip replacement: Stryker MAKO robotic assisted with Accolade II and Tritanium implants.
Mears SC: Outcomes of displaced and nondisplaced pelvic and sacral fractures in elderly adults. J Am Geriatr Soc 2011, 59
Hopf JC: Percutaneous iliosacral screw fixation after osteoporotic posterior ring fracture of the pelvic reduces pain significantly in elderly patients. Injury, 2015, 46, 1631
Author: Professor Peter Biberthaler MD.
Institution: Technical University of Munich, Klinikum rechts der Isar, Munich, Germany.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















