Vein sheathing repair of a cutaneous nerve and EPL tendon repair
Overview
Subscribe to get full access to this operation and the extensive Upper Limb & Hand Surgery Atlas.
Watch the overview
Learn the Vein sheathing repair of a cutaneous nerve and EPL tendon repair surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Vein sheathing repair of a cutaneous nerve and EPL tendon repair surgical procedure.
Open hand injuries can result from a variety of mechanisms including sharp objects, commonly glass or knife or from power tools. When assessing these patients, it is important to be systematic to identify all structures which are injured. When planning the exposure allowance should be made consider the possibility that certain tendons such as EPL can retract significantly into the forearm and the exposure may need to be extended proximally. Glass injuries are common in the hand and tend to be deep and at risk of structural injury, even if the lacerations appear small.
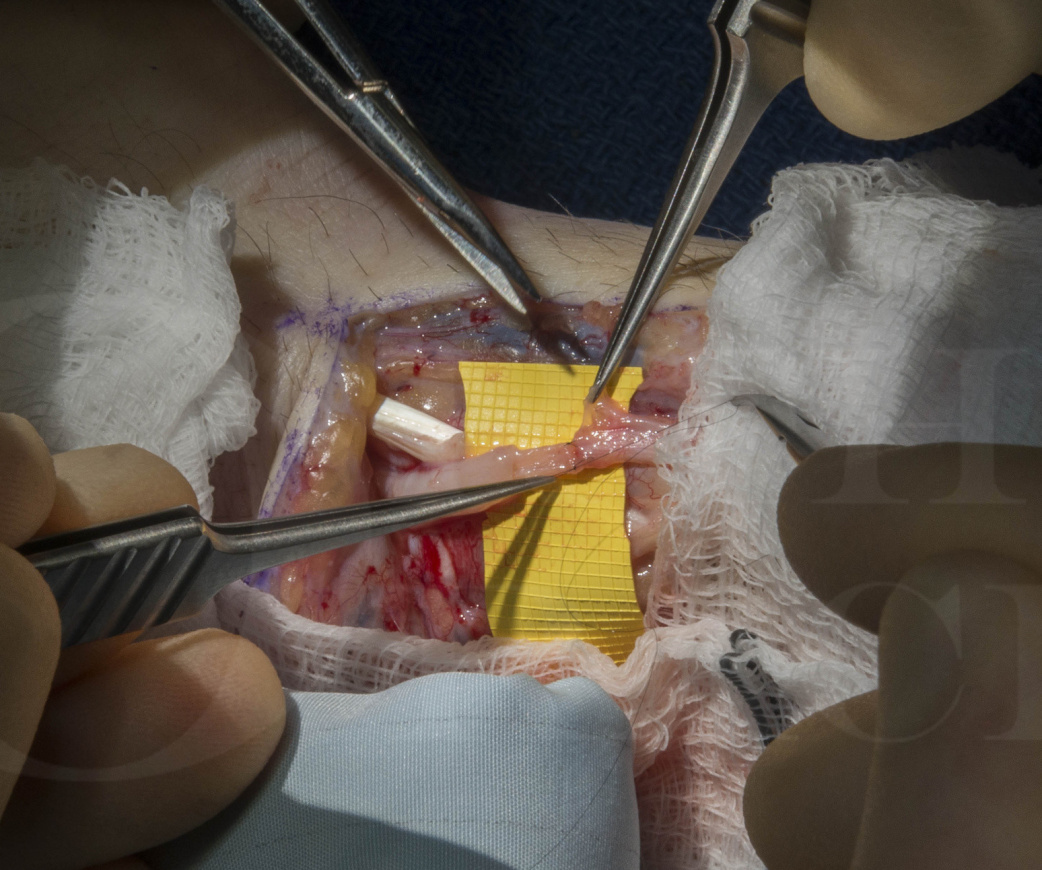
The patient in this case sustained lacerations to the dorsum of the hand with a broken glass which divided the extensor pollicis longus tendon and superficial radial nerve. Superficial sensory nerve repairs in the upper limb can be complicated by the development of neuromas and perineural scarring. This is particularly a problem on the dorsum of the hand where there is less subcutaneous tissue, and the sensitised nerves can cause neuropathic pain on even light pressure. I have adopted a technique of sheathing the nerves during their primary repair to reduce the risk of this painful scarring. In a comparative study of neurorrhaphy with and without vein sheathing Leuzzi and co-authors found that 70% of simple neurorrhaphy patients reported pain at the nerve repair site whereas it dropped to 25% when vein sheathing was used.
For most cutaneous nerves, an adjacent vein can be sacrificed for wrapping around the nerve repair. For example, for the superficial radial nerve and lateral cutaneous nerves of the forearm the cephalic vein or its branches can be used. For the medial cutaneous nerve of the forearm or the dorsal branch of the ulnar nerve the basilic vein can be used. It is an anatomical fact that superficial sensory nerves accompany veins, which lends itself to this technique. There are no side effects to sacrificing a cutaneous vein as there are several superficial and deep veins which compensate for the function lost.
There are also commercial nerve wraps available as alternatives, but these are expensive and have no real advantage over autologous veins for protecting small nerve repair. I tend to use the commercial nerve wraps for larger nerves, such as the median or ulnar nerve, when they are released from scar tissue as a secondary procedure. This is because the cutaneous veins of the upper limb are not large enough to be wrapped around larger nerves without causing constriction.
Readers will also find the following OrthOracle techniques of interest:
Targeted muscle re-innervation for superficial radial neuroma
Targeted Muscle Reinnervation (TMR) for neuroma treatment following above knee amputation
Revision carpal tunnel decompression and application of Polyganics Vivosorb membrane
Digital nerve conduit-assisted repair with the NeurolacTM (Polyganics)
Leuzzi S, Armenio A, Leone L, et al. Repair of peripheral nerve with vein wrapping. G Chir. 2014;35(3-4):101-106.
Author: Rajive Jose FRCS
Institution: The Queen Elizabeth Hospital, Birmingham, UK.
Clinicians should seek clarification on whether any implant demonstrated is licensed for use in their own country.
In the USA contact: fda.gov
In the UK contact: gov.uk
In the EU contact: ema.europa.eu



















